Recruiting, Ongoing, Upcoming, & Completed Studies
Conducted between 2021-2026
Predominately funded by NIH grants U19-DE-28717 and U01-DE-28727
Studies for which data collection has ended (n=19)
Study PI: Dr. Jin Xiao, Eastman Institute for Oral Health University of Rochester Medical Center
Study PI: Dr. Dorota Kopycka-Kedzierawski, Eastman Institute for Oral Health University of Rochester Medical Center
Brief Study Description
Amid the COVID-19 outbreak, dentistry urgently needs modified dental examination regimens that render quality care and ensure the safety of patients and the dental health care personnel (DHCP). Traditional dental examinations – more than 300 million per year in the US – rely on person-to-person visual-tactile examination, posing challenges to infection control and consuming large quantity of advanced level personal protective equipment (PPE).
Our long-term goal is to develop an innovative mDentistry (mDent) model. This model supplements the traditional practice of dentistry with virtual visits supported by mobile devices such as mobile phones, tablets, personal digital assistants, and the wireless infrastructures. The mDent leverages advantages of virtual dental visits and digital mHealth tools, such as intraoral cameras, to deliver virtual oral examinations, treatment planning, and interactive oral health management on a broad population basis.
This mDentistry (mDent) eHygiene study is the first step of utilizing the mDentistry model, which will access the rich resources of the National Dental Practice-Based Research Network, recruit 24 DHCP (Dentists and Hygienists) and 144 patients from practices across regions of the Network, and assess the acceptance of virtual dental examinations by patients and the dental health care personnel. The mDentistry eHygiene model has the potential of empowering patients with mhealth tools and engaging them in oral health care delivery.
Study results will inform of immediate modification of the dental service system, provide safe care delivery, and preserve PPEs amid COVID-19 pandemic.
Key study publications:
Xiao J, Kopycka-Kedzierawski D, Ragusa P, Mendez Chagoya LA, Funkhouser K, Lischka T, Wu TT, Fiscella K, Kar KS, Al Jallad N, Rashwan N, Ren J, Meyerowitz C; National Dental Practice-Based Research Network (PBRN) Collaborative Group. Acceptance and Usability of an Innovative mDentistry eHygiene Model Amid the COVID-19 Pandemic Within the US National Dental Practice-Based Research Network: Mixed Methods Study. JMIR Hum Factors 2023;10:e45418.
Xiao J, Meyerowitz C, Ragusa P, Funkhouser K, Lischka TR, Chagoya LAM, Wu TT, Fiscella K, Ivie E, Strange M, Kopycka-Kedzierawski DT, National Dental Practice Based Research Network Collaborative Group. Assess an innovative mDentistry eHygiene model amid the COVID-19 pandemic in the National Dental Practice Based Research Network: protocol for design, implementation, and usability testing. JMIR Research Protocols 2021; 10(10)e32345.
Because of the small number of practitioners and patients in this study and the fact that they were all from a limited geographic area, it is not possible to provide a de-identified data set that does not risk being identifiable. Therefore, no public use data set is available.
Self-Contamination of PPE Study
Study PI: Dr. Jennie Kwon, Washington University
Brief Study Description
The Occupational Health and Safety Administration (OSHA) places dental healthcare providers (DHCP) in the very high exposure risk category for being exposed to SARS-CoV-2, the virus that causes COVID-19. However, data regarding the transmission dynamics of infectious agents in dental settings is limited, and studies evaluating methods to prevent organism transmission in dentistry are urgently needed. DHCPs regularly interact with patient saliva, which has high viral loads of SARS-CoV-2 in infected patients. Although it is discouraged to perform procedures on individuals with active COVID-19, epidemiologic data indicates that there are individuals who asymptomatically carry SARS-CoV-2. Thus, appropriate personal protective equipment (PPE) is necessary to protect DHCPs from SARS-CoV-2. However, data regarding the transmission of infectious agents when utilizing PPE in the dental setting is limited. Most transmission dynamics studies regarding PPE use were performed in the hospital setting; however, DHCPs have different and specific needs than that of a hospital healthcare provider. The purpose of this proposal is to identify potential routes of self-contamination during PPE donning and doffing by DHCPs using a fluorescent marker as a surrogate for pathogen transmission, and pilot an educational video focused on improving PPE donning and doffing techniques.
Key study publications:
Vogt LC, Reske KA; Park D, Bach TH, Stewart HB, Arter OG, Stoeckel D, Steinkamp HM, Liang SY, Durkin MJ, Kwon JH. Personal protective equipment use among dental healthcare personnel during COVID-19 and impact of an educational video in clinical practice. Infection Control & Hospital Epidemiology 2023;44(9):1472-1480.
Reske KA; Park D, Bach TH, Stewart HB, Vogt LC, Arter OG, Stoeckel D, Steinkamp HM, Liang SY, Durkin MJ, Kwon JH. Assessment of dental health care personnel protocol deviations and self-contamination during personal protective equipment donning and doffing. Journal of the American Dental Association 2022; 153(11):1070-1077.
Study PI: Dr. Sydnee Chavis, University of Maryland School of Dentistry
Brief Study Description
Patients with special healthcare needs (SHCN) face significant barriers to dental care compared to the general population. A significant proportion of these barriers has been demonstrated to stem from lack of practitioner training and education in the context of the care for patients of this population. However, methods of addressing practitioner training and remedying these barriers to care have not been extensively studied. Similarly, the attitudes of dental practitioners regarding treatment of patients with SHCN of all ages have not been studied across dental specialties in a community-based setting. This national questionnaire study seeks to ascertain perspectives and attitudes of dental practitioners regarding the care of patients with SHCN, as well as practitioner training and educational experiences regarding the care and management of patients with SHCN across the lifespan. The study will also seek to identify the methods that practitioners do utilize in practice to treat patients with SHCN in the community setting. The specific aims for this study are to:
- Identify the practitioner and practice based factors that influence treatment of patients with SHCN.
- Identify and quantify the methods, procedures, and protocols practitioners utilize to provide dental care for patients with SHCN.
The National Dental Practice-Based Research Network (PBRN) provides a forum for a target population that has not previously been studied regarding the care they provide for patients with SHCN. It is a unique and innovative forum to explore community-based practitioner perspectives and methods of treatment for patients with SHCN. This project will serve to provide preliminary data regarding reasons dental practitioners in the community do or do not provide care for patients with SHCN, how this relates to their educational and training experiences with patients of this population, and the methods of practice that are utilized in practice for this population, which will be utilized to develop targeted educational and training content to be further distributed and tested within the National Dental PBRN.
Key study publications:
In development.
Study data dictionary [will provide after main results have been accepted for publication]
Data set [will provide after main results have been accepted for publication]
Study PI: Dr. Jeffrey Fellows, Kaiser Permanente Northwest Center for Health Research
Brief Study Description
The proposed “Coronavirus Acceptability and Readiness Among Dentists (CARAD)” study uses a mixed-methods approach to evaluate dentists’ interest and ability to participate in a SARS-COV-2 delivery program. This CARAD study will be conducted with adult dental patients and dentists enrolled in the Western Region of the National Dental Practice-Based Research Network (PBRN). The objectives of the proposed study include:
- Analyze the acceptability, appropriateness and feasibility of a dental office-based SARS-CoV-2 program among adult patients following offer at a routine dental office visit.
- Analyze the acceptability, appropriateness and feasibility of adopting a SARS-CoV-2 delivery program among dental practitioners with existing program experience.
- Assess levels of acceptability and readiness to participate in a SARS-CoV-2 delivery program through dental offices, by dentists and practice characteristics, and accounting for relevant supply management and legislative factors.
Key study publications:
Gruß I, Papajorgji-Taylor D, Tommasi NP, Pihlstrom DJ, Hendrickson BP, Ikeda J, Manning W, Madden T, Jeffrey L. Fellows. Dental providers’ perceptions of the feasibility and acceptability of implementing administration programs in dental settings: A qualitative study. Journal of Public Health Dentistry 2022; 82(3):330-337.
Fellows JL, Smith N, Laws R, Gruss I, Papjorgi-Taylor D, Pihstrom D, Henderickson B, Madden T, Manning W, Ikeda J, McBurnie MA, Crawford P, Hu W, Mathur S, Gilbert GH, for the National Dental PBRN Collaborative Group. Dentist’s personal and professional attitudes about delivery. AADOCR annual meeting. Portland, OR. March 15-18, 2023. Abstract 3817124.
Study PI: Dr. Michael Durkin, Washington University
Brief Study Description
Our long-term goal is to develop a comprehensive evidence-based infection prevention toolkit to protect dental health care personnel (DHCP) and patients. This includes identifying the highest risk dental procedures, determining the appropriate PPE to wear for dental procedures, and instructing dentists how to appropriately don and doff PPE (including gowns, gloves, masks, and eye protection). Our study goals are to characterize the organic and inorganic composition of dental aerosols as a surrogate marker to assess the clinical risk of COVID-19 for DHCPS. We believe that such work will better quantify risks, differentiate bacterial pathogens disseminated via splatter from large droplets vs. Aerosols, and inform future mathematical modeling experiments.
Aim 1: Evaluate the organic composition of dental aerosols
Aim 1a: Evaluate bacterial burden of dental aerosols
Aim 1b: Evaluate viral composition of dental aerosols
We will use a combination of several sensors to simultaneously capture the size and biologic composition of dental aerosols. We plan to perform analyses on low- and high-risk dental procedures. Bacterial and viral samples with be processed, frozen, and stored for batched testing. Bacterial specimens will be sent for routine bacterial culture in a microbiology laboratory. Viral testing will be performed using the combination Biofire FilmArray Respiratory Panel and SARS-CoV-2 RT-PCR test. This approach will allow the study team to capture detailed data on the biological contents of dental aerosols.
Aim 2: Evaluate the inorganic composition of dental aerosols
We will perform inorganic chemical analysis of dental aerosols. This will provide us with a second approach to explore the dilutional effect of aerosols in water cooled equipment. Furthermore, this analysis will aid with evaluation of occupational health exposures DHCPs may receive via aerosolization of enamel, dentin, and amalgam materials.
Key study publication:
Choudhary S, Bach T, Wallace MA, Stoeckel DC, Thornhill MH, Lockhart PB, Kwon JH, Liang SY, Burnham CD, Babcock HM, Biswas P, Steinkamp HM, Durkin MJ. Assessment of infectious disease risks from dental aerosols in real world settings. Open Forum Infectious Diseases 2022; 9(11):ofac617.
Study PI: Dr. Michael Durkin, Washington University
Brief Study Description
Little is known regarding aerosol generation during dental procedures. This information is critical to help dental healthcare personnel make evidence-based decisions regarding appropriate personal protective equipment (PPE) use in dental clinics. The purpose of this proposal is to quantify aerosol formation during common dental procedures and evaluate current non-evidence-based strategies employed in dental settings to reduce aerosolization.
Our multidisciplinary team includes environmental engineers from Washington University in St. Louis who will quantify particle size, concentration, and duration in real world dental settings; infectious diseases and infection prevention experts from Washington University School in St. Louis of Medicine who will interpret the data; dental partners, including St. Louis University Center for Advanced Dental Education and community clinics, which will serve as collaborating sites; and international leaders in dental research who will serve as dental content experts.
At the end of this grant, our team will provide pragmatic guidance to dentists regarding optimal PPE (e.g., surgical mask vs N95 respirator or equivalent) for a variety of common dental procedures. Furthermore, our team will determine the impact of a variety of aerosol mitigation interventions on particle size and quantity in real world dental settings.
Key study publication:
Choudhary S, Durkin MJ, Stoeckel DC, Steinkamp HM, Thornhill MH, Lockhart PB, Babcock HM, Kwon JH, Liang SY, Biswas P. Comparison of aerosol mitigation strategies and aerosol persistence in dental environments. Infection Control and Hospital Epidemiology 2022; 43:(12):1779-1784.
Study PI: Dr. Jeffrey Fellows, Kaiser Permanente Northwest Center for Health Research
Brief Study Description
The spread of the novel coronavirus, SARS-CoV-2 (SC2), has currently infected over 1.7 million Americans with COVID-19 and caused over 100,000 US deaths. The pandemic has severely impacted healthcare delivery systems, economic activity, and social relationships. In March 2020, most states temporarily postponed non-emergency oral healthcare services to reduce exposure to the disease and to conserve personal protective equipment (PPE) for hospital care. Many dental procedures generate substantial aerosols, droplets, and fomites. Beginning in late April, states began allowing dental offices to reopen for routine care services. However, the incidence of COVID-19 and related deaths are increasing in the US, with considerable variation by state and county. Public health agencies and professional organizations have published general practice recommendations for dental care and are expected to evolve as we learn more about this novel coronavirus. Dental practitioners may use different approaches and combinations to reduce SC2 transmission, including modifications to facilities, patient flow, dental procedures and delivery methods, and personal protective equipment (PPE).
This study establishes a National Dental PBRN COVID-19 REsearch (CORE) Registry to support multilevel intervention and implementation science research on topics that are important to dental practitioners that include factors at the environmental, organizational, and/or individual level. We will recruit about 2,000 active National Dental PBRN practitioners to participate in the CORE Registry study. The objectives of the proposed CORE Registry are to: a) identify effective approaches used by National Dental PBRN practitioners to mitigate SC2 transmission risks, their costs, and assess practitioners’ comfort levels with these approaches; b) disseminate and discuss effective combinations of mitigation methods with participating practitioners and evaluate the impacts of these activities on the use of effective mitigation approaches and comfort levels, accounting for other factors; and d) establish a modular infrastructure to support the design and conduct of additional multilevel clinical and implementation science research. Classification and Regression Tree techniques are used to evaluate study objectives, overall and by practice setting, location, and specialty.
Key study publication:
Fellows JL, McBurnie M, Laws R, Allareddy V, Leo M, Law A, Nosrat A, Machen C, Mathur S, Shaw D, Crawford P, Hu W, for the National Dental PBRN Collaborative Group. Impact of SARS-CoV-2 on the sustainability of dental practice: National Dental PBRN. Presentation at the 2022 AADOCR Annual Meeting. Atlanta, GA. March 24, 2022. Abstract 3666291.
Study PI: Dr. Omid Amili and Dr. Choueiri, University of Toledo
Brief Study Description
In modern dental care procedures, aerosols and droplets are generated from the use of high speed handpieces, ultrasonic scalers, and other dental care equipment. This naturally puts both the patients and the dental care providers at a higher risk of respiratory infection due to the presence of higher levels of potentially contaminated droplets and particulate matters in dental offices. In this experimental study, we propose to develop a robust platform to fully assess the air quality in dental settings and develop recommendations for immediate and long-term adjustments necessary to minimize the transmission of highly infectious respiratory diseases such as COVID-19.
This project is designed to achieve three specific aims. First, we develop a respiratory patient simulator to generate and characterize a physiologically accurate cloud of droplets and aerosols. The experimental simulator will be furnished with particle image velocimetry capabilities as well as pressure, temperature, humidity, and particle sizer/counter sensors. This portable and versatile rig will enable us to carry out a benchmark study under well controlled laboratory conditions in order to generate and characterize the behavior of expelled particles resulting from the most common dental procedures as well as expiratory events. Second, we characterize the particle topography and size distribution during various dental procedures using air-turbine handpieces and air-water syringe sprays while a dentist performs these procedures on the patient simulator. We will fully characterize the particle distribution as a function of a large parameter space including the common dental treatments, patient’s posture, office layout, and air conditioning system settings, all in the absence of human subjects but with a dentist operating on the dental typodont of the respiratory simulator. Third, we quantify the map of particle topography and size distribution under modified work conditions. We will use barriers such as flexible face shields and an external oral suction device among other respiratory droplet protective/preventive equipment to reduce the transport of aerosols and droplets in dental offices. Imaging and point measurements will be performed under the altered/modified work conditions in the same parameter domain as in the second aim to characterize the change in particle concentration, accumulation, and dissipation over time.
This study will identify the most hazardous particle concentration locations with respect to the patient/dentist and will reveal the most effective operation conditions and room layouts (open semi-open/closed) to provide specific recommendations for the reduction of aerosol/droplet transmission. We will investigate the spatio-temporal correlation of the particle size and concentration in different locations of the testing area over time. In a broader scope, this project provides us the opportunity to improve our understanding of the transport of dense clouds of particulate matters (in both liquid and solid forms) applicable to a wider array of respiratory related questions. In addition, this platform enables us to develop and test respiratory protective equipment using a range of physiologically accurate aerosols and droplets.
Key study publication:
Dabiri D, Conti SR, Pour NS, Chong A, Dadjoo S, Dabiri D, Wiese C, Badal J, Hoogland MR, Conti HR, Taylor TR, Choueiri G, Amili O. A multi-disciplinary review on aerobiology of COVID-19 in the dental setting. Frontiers in Dental Medicine 2021; 2: 726395.
The full study protocol used, including design, data acquisition, and data processing procedures, are available at these two locations:
The data set is large, but available from the Study PI by email Dr. Amili at [email protected]
Study PI: Cecile Feldman, DMD, MBA
Brief Study Description
This project is designed to develop practice protocols that address the safety of patients and dental health personnel in a COVID-19 environment.
This study will use experts drawn from science, industry (insurance), practice (dentistry) and patients (community) to identify areas concerning office safety and security in a COVID-19 world and develop new ways of approaching dental practice that insures a sense of security and practicality for both patients and health professionals. After a consensus is developed, two to three new practice models that incorporate these recommendations will be put forward for testing to obtain pilot data. These methodologic improvements in dental practice will be based on the most current scientific knowledge and will be pragmatically applied to ensure safety in a dental office setting.
The specific aims of this proposal are divided into three parts. The first aim is to assemble a panel of experts and stakeholders to engage in a Delphi process. Weaknesses in current COVID dental practice guidelines will be identified along with consequential pragmatic and novel methodological changes. The investigative team will then present these pragmatic changes to the Delphi group to gain their approval and/or recommended modifications. The second aim is to develop two to three guidelines for improvement of dental office practices that can be tested within the framework of the PBRN to assess acceptability, safety, effectiveness and efficiency in a dental office setting. Our third aim is to finalize the planning for a PBRN based study to fully test out these strategies and whose results are generalizable. To achieve this, a pilot study to test the most promising pragmatic/innovative modifications will be conducted in 4 to 6 PBRN based practices. The pilot will assist in finalizing study methodology, protocol and data collections instrument development, and complete sample size calculations.
Ultimately, this research will enable dental health care workers to safely return to work, providing essential oral health care services in the best possible environment. It will provide patients with confidence that they could resume seeking dental care under optimal conditions that insures their well-being.
Key study publications:
Fredericks-Younger J, Feldman C, Fine DH, Subramanian G, Gennaro ML, Coker M, Meyerowitz C, , Allareddy V, Funkhouser E, McBurnie MA, Ragusa P, Chapman-Greene J. Pragmatic return to effective dental infection control through triage and testing (PREDICT): an observational, feasibility study to improve dental office safety. Pilot and Feasibility Studies 2024; 10(1):44.
Feldman CA, Fredericks-Younger J, Fine D, Markowitz K, Sabato E. Advancing oral health through practice-based research. Journal of the American Dental Association 2023; 154(11): 959-962.
Coker MO, Subramanian G, Davidow A, Fredericks-Younger J, Gennaro ML, Fine DH, Feldman CA. Impact of DHCW’s safety perception of risk mitigation strategies. JDR Clinical and Translational Research 2023; 8(2):188-197.
Fredericks-Younger J, Fine DH, Subramanian G, Coker MO, Meyerowitz C, Ragusa P, Allareddy V, McBurnie MA, Funkhouser E, Gennaro ML, Feldman CA. The pragmatic return to effective dental infection control through triage and testing (PREDICT) study: protocol for a prospective clinical study in the National Dental Practice-Based Research Network. JMIR Research Protocols 2022; 11(8):e38386.
Feldman CA, Fredericks-Younger J, Subramanian G, Gennaro ML, Coker MO, Fine DH. Severe acute respiratory syndrome coronavirus 2 screening to augment dental office and patient safety. Journal of the American Dental Association 2022: 153(5):399-402.
Because of the small number of practitioners and patients in this study and the fact that they were all from a limited geographic area, it is not possible to provide a de-identified data set that does not risk being identifiable. Therefore, no public use data set is available.
Deep Caries Removal Strategies Study (DCS)
Study PI: Dr. Marianne Jurasic, Boston University
Brief Study Description
Dental caries is a preventable disease; however, it still affects large numbers of people globally and in the US. The expectation is that untreated caries will continue to rise as the aging population increases and the edentulous rate decreases. Current evidence suggests that less invasive treatment should be employed that can preserve hard tissue and retain teeth long term. Nevertheless, disparity in the management of deep carious lesions remains. The purpose of this study is to survey National Dental PBRN dentists regarding their treatment practices for managing deep carious lesions and assess their willingness and ability to participate in a randomized controlled trial evaluating deep caries removal strategies in permanent teeth in adults (18+).
Key study publication:
Jurasic MM, Gillespie S, Sorbara P, Clarkson J, Ramsay C, Nyongesa D, McEdward, D, Gilbert GH, Vollmer WM for the National Dental PBRN Collaborative Group. Deep caries removal strategies: findings from the National Dental PBRN. Journal of the American Dental Association 2022; 153(11):1078-1088.
Study PI: Dr. Sharon Elad, University of Rochester
Brief Study Description
Dental intervention-related oral bleeding is an important consideration when treating patients on anticoagulants (ACs). The literature reports of extensive bleeding complications in patients on warfarin affecting 1.5-26% of the patients. The prevalence of minor bleeding is reported within the range of 3-9.7%. Several societies have published guidelines on how to minimize the risk for bleeding in patients receiving ACs, however, the rapidly emerging new anticoagulants pose new challenges with limited clinical data from the US.
The overall goal of the study is to assess the current understanding and approach of dental practitioners about the management of patients on anticoagulants, including conventional and direct oral anticoagulants (DOACs) in practice.
By surveying approximately 1,650 members of the National Dental Practice-Based Research Network, the survey will look into common tendencies and practices regarding dental treatment for patients on anticoagulants by practitioners across the United States. The information generated from the study will help in understanding the gaps in clinical practice regarding the management of anticoagulated patients, which will assist in development and implementation of guidelines for the treatment of patients on ACs, particularly DOACs, in the dental practice.
Key study publication:
Elad S, Connolly G, Cacciato R, Boy R, Leo M, Calnon W, Gillespie-Crawford S, Gilbert GH, Meyerowitz C. Classification of bleeding severity by general dentists in the National Dental Practice-Based Research Network: a survey-based assessment. Quintessence International 2025; 56(8):668-679.
This study was funded by U01-FD-005938, not U19-DE-28717. Consequently, the responsibility for public access to data from this study lies with that grant.
Study PI: Yale-Mayo Clinical Center of Excellence in Regulatory Science (CERSI)
The study’s specific aims were to examine: (1) patients’ pain trajectories in episodes of acute pain for which opioids were prescribed, tracking pain severity and persistence, as well as prescribed and over-the-counter pain medication use; (2) associations between patient demographic, clinical and emotional characteristics and pain and opioid use trajectories; and (3) how patients handled unused opioids.
Key study publications:
Jeffrey MM, Bellolio F, Allen S, Fillmore WJ, Gilbert GH, Heckman R, Lipkind H, Elie M-C, Nuckols TK, Ritchie JD, Page D, Wallace D, Walter L, Tamang S, Torbati S, Chang N, Zhao Y, Pacanowski MA, Soukup M, Lee C, Meyer TE, Mallama C, Shah ND, Ahadpour M, Koussis P, Ross JS. Opioid use and pain resolution for acute pain among opioid-naïve patients. JAMA Network Open 2026; accepted for publication.
Jeffery MM, Ahadpour M, Allen S, Araojo R, Bellolio F, Chang N, Ciaccio L, Emanuel L, Fillmore J, Gilbert GH, Koussis P, Lee L, Mallama C, Meyer T, Moncur M, Nuckols TK, Pacanowski MA, Page DB, Papadopoulos E, Ritchie J, Ross JS, Shah ND, Soukup M, St. Clair CO, Tamang S, Wallace DW, Zhao Y, Heckmann R. Acute Pain Pathways: protocol for a prospective cohort study. BMJ Open 2022; 12(7):e058782.
This study was funded predominately by R01-HS-025177, not U19-DE-28717. Consequently, the responsibility for public access to data from this study lies with that grant.
Study title: Dental prescribing of antibiotics and opioids: high use in the absence of evidence
Study PI: Katie J. Suda, PhD; University of Illinois at Chicago (now at University of Pittsburgh)
Brief Study Description
Antibiotics and opioids are the top therapeutic categories prescribed by dentists. There is a current knowledge gap in our understanding of medication prescribing and overprescribing (inappropriate indications and/or excessive quantity/potency/duration) by dentists. This gap is significant because dentists prescribe 1 out of every 10 prescriptions for both antibiotics and opioids in the US. Although efforts are increasing to curtail inappropriate use of these medication classes, most interventions are focused on physicians and midlevel providers (nurse practitioners, physician assistants). Guided by preliminary data, we will pursue two specific aims: 1) Assess dental prescribing of antibiotics and opioid medications and identify patient and prescriber characteristics associated with high rates of overprescribing and 2) Compare attitudes to- wards prescribing antibiotics and opioids for dentist with practices located in high and low prescribing com- munities across the United States.
We propose to conduct a mixed-methods study to assess antibiotic and opioid dental prescribing based on American Dental Association treatment recommendations and identify factors related to prescribing. The expected outcomes of this study include providing baseline data on the extent of antibiotic and opioid overprescribing by dentists, identification of barriers and facilitators to improving prescribing of antibiotics and opioids and selection of a pilot implementation project to improve the quality of dental care.
Key study publications:
Ramanathan S, Yan C, Suda KJ, Evans CT, Khouja T, Hershow RC, Rowan SA, Gross AE, Sharp LK, National Dental PBRN Collaborative Group. Barriers and facilitators to guideline concordant dental antibiotic prescribing in the United States: a qualitative study of the National Dental PBRN. Journal of Public Health Dentistry 2024; 84(2):163-174.
Yan CH, Ramanathan S, Suda KJ, Khouja T, Rowan SA, Evans CT, Lee TA, Calip GS, Gellad WF, Sharp LK, National Dental Practice-Based Research Network Collaborative Group. Barriers and facilitators to opioid prescribing by dentists in the United States: a qualitative study. Journal of the American Dental Association 2022; 153(10):957-969.
Mental health Screening and referral in Dental Practices (MSDP)
Study PI: Dr. Blake Berryhill, Dr. Nathan Culmer, Dr. Todd Smith
Brief Study Description
The purpose of this study is to collaborate with dental offices in the National Dental PBRN to develop and evaluate procedures for integrating mental health screening and procedures into dental care workflows. Nearly one in five U.S. adults has struggled with mental illness in the last year and yet over half of those individuals did not receive treatment during that time – necessitating improved screening and referral networks for mental health. Given that people may see their dentists more often than their primary care physician, and that changes in mental health can occur rapidly and dramatically, equipping dentists to screen for mental health issues is necessary and urgent. A network Quick Poll conducted in 2018 found that nearly 93% of dentists understand that dental and mental health are related. Our long-term goal is to develop standardized implementation procedures for integrating mental health screening and referral to treatment procedures in dental offices. In this application, our overall objectives in support of that long-term goal are to: 1) identify potential implementation barriers and facilitators for integrating mental health screening and referral to treatment procedures into network dental practices; 2) develop mental health screening and referral to treatment procedures into network practices’ workflows; and 3) evaluate the feasibility of integrating mental health screening and referral to treatment procedures into the dental health workflow using a pilot study involving network practices. Our project team will use our expertise in dentistry, mental health, medicine, practice management, training, evaluation and research to develop, integrate, and evaluate the implementation of mental health screening and referral procedures into dental workflows. The viability of this proposal is supported by the fact that increased experience with mental health among dentists is associated with increased likelihood of discussing mental health concerns with patients and referring them to mental health treatment when appropriate and that integration of screening and referral procedures will increase the accuracy and likelihood of such discussions and referrals. Thus, developing and integrating mental health screening and referral mechanisms into dental practice workflows, and subsequently piloting and evaluating feasibility of procedures, is expected to expand patient access to mental health resources. By screening more adults for mental health issues and building connections to mental health resources in their area, dentists contribute meaningfully to the overall well-being of their patients and increase access to mental health care in their communities. At project completion, we expect have the outcome of an adaptive, refined set of procedures for implementing mental health screenings and referrals into dental practices. By integrating mental health more comprehensively into dental practices, results will enable us to pursue our overall goal of pursuing a larger scale trial, which ultimately advances the mental health care needs of dental patients.
Key study publications:
Berryhill MB, Culmer N, Smith TB, McBurnie MA, Barton D, Machen C, Kopycka-Kedzierawski D, Gilbert GH. Patient perceptions on the acceptability and appropriateness of mental health screening and follow-up in National Dental PBRN practices. Translational Behavioral Medicine 2025; 15(1):ibaf022.
Smith T, Berryhill MB, Culmer N, McBurnie MA, Kopycka-Kedzierawski D, Gilbert GH, Barton D, Machen C. Mental health screenings in dental settings: feasibility and outcomes from a National Dental PBRN study. Journal of the American Dental Association 2024; 155(11):963-971
Berryhill MB, Culmer N, Smith T, Kopycka-Kedzierawski DT, Gurganus R, Curry G. Perceptions of mental health screening and referral to treatment in National Dental PBRN practices: a qualitative study. Journal of Public Health Dentistry 2024; 84(2):124-135.
Because of the small number of practitioners and patients in this study and the fact that they were all from a limited geographic area, it is not possible to provide a de-identified data set that does not risk being identifiable. Therefore, no public use data set is available.
Study PI: Dr. Jenna McCauley
Brief Study Description
This study aims to identify critical training and implementation gaps in performing substance use (including tobacco/nicotine, alcohol, prescription misuse, and illicit drugs) screening among adolescent, young adult, and adult patients in dental offices/practices. This study consists of an online survey of member dentists regarding their current knowledge, training experiences, and practice behaviors related to substance use screening of patients. Data from the survey will be paired with key practice-related enrollment data to identify implementation gaps and whether these gaps vary by practice/practitioner characteristics, as well as to inform the development of training and interventions targeting enhanced substance use screening and early intervention in dental practices.
Key study publications:
McCauley JL, Crawford P, Leo MC, McBurnie MA, Barton D, Weidner HA, Rindal DB, National Dental PBRN Collaborative Group. Dental screening, counseling, and referral to treatment for substance use disorder: survey of the National Dental Practice-Based Research Network. Journal of Studies on Alcohol and Drugs 2026; 87(1): 54-63.
McCauley JL, Leo MC, Crawford PM, McBurnie MA, Barton DM, Weidner HA, Rindal DB, National Dental PBRN Collaborative Group. Willingness to provide naloxone: survey of the National Dental Practice-Based Research Network. Journal of Opioid Management 2025; 21(6): 543-550.
McCauley JL, Leo MC, Crawford P, McBurnie MA, Barton DM, Weidner HA, Rindal DB, Gilbert GH. Substance use screening among adolescents: National Dental Practice-Based Research Network survey. Journal of Adolescent Health 2025; 77(6):1088-1096.
Post-Operative Pain Study (POPS)
Study PI: Muhammad Waji, PhD
Brief Study Description
Pain is a common, and unwelcome aftermath of seeing the dentist. Indeed, pain has been deemed the fifth vital sign and many describe it as an adverse event (AE). After the effects of the most commonly-used local anesthetic diminishes, dental patients must rely on themselves and their own understanding for pain management following dental procedures. This has led to an over-reliance on prescribed opioids as there are no means to actively track patients’ pain once they leave the clinic. To understand effective/appropriate pain management, we need to examine the pain levels experienced by patients caused by which dental procedures. Such an inventory will allow providers to anticipate and better manage their patients’ post-operative pain.
Innovative mobile applications and connected health technologies that allow real-time tracking of patients’ symptoms, functional status and quality of life, provide healthcare professionals with data that were previously unavailable, and have fostered patient engagement, shared decision-making and adherence to treatment plans. We propose to explore an innovative solution to dental pain monitoring and management by implementing mobile phone technology to monitor patients’ pain during the critical acute post-operative phase.
We believe that by tracking patient reported outcomes (PROs) using mobile phones, patients with sub-optimal pain experiences will be easily identified. This study will demonstrate that PROs provide actionable data. This study can also serve as a model for implementing new health IT (mHealth) within dental practices to improve patient engagement.
This observational study will be conducted at the National Dental Practice-based Research Network (the Network) sites, which we believe are ideal for the development of this practical and focused post-operative pain management study. We will recruit up to 50 Network practices and 4050 patients who will receive push notifications through text messages using FollowApp.Care on their mobile phones at designated time intervals following their dental procedure. This innovative approach of implementing an existing and tested mHealth system technology (FollowApp.Care) into the real-world dental office setting of the Network will actively track pain and other complications following dental procedures. By patients using their mobile phones, we expect to promptly and precisely identify specific levels of pain for surgical dental procedures.
During the UG3 phase of the study (Yr 1-2) we will develop all study materials in UG3-Aim1, and in UG3-Aim 2 develop the design features and workflow for implementation of the study. During the UH3 phase (Yr 3-6) we will in UH3-Aim1, pilot test procedures to streamline data collection and workflow in the Network dental office. In UH3- Aim 2 we will assess post-operative pain intensity by procedure type; in UH3-Aim 3 we will assess provider and patient post-op management strategies and in UH3-Aim 4, we will evaluate patients’ and providers’ acceptance of the mHealth technology.
Key study publications:
Walji MF, Yansane A-I, Tungare S, Mungia R, Holmes D, Funkhouser K, Machen C, Urata J, Redlund C, Shirodkar G, Malmstrom H, Yu DH, Tokede O, Rindal DB, Gilbert GH, Spallek H, White JM, Kalenderian E, National Dental PBRN Collaborative Group. Postoperative pain after dental procedures: The National Dental PBRN observational study using a mobile health platform. Journal of the American Dental Association 2026; in press.
Kalenderian E, Tungare S, Mehta U, Hamid S, Mungia R, Yansane A, Holmes D, Funkhouser K, Ibarra-Noriega A, Urata J, Rindal DB, Spallek H, White J, Walji M. Patient and dentist perspectives on collecting patient reported outcomes after painful dental procedures in the National Dental PBRN. BMC Oral Health 2024; 24(1):201.
Kalenderian E, White J, Yansane AI, Urata J, Holmes D, Funkhouser K, Mungia R, Xiao J, Rauschenberger C, Ibarra-Noriega A, Tran D, Rindal DB, Spallek H, Walji M. Study protocol: understanding pain after dental procedures, an observational study within the National Dental PBRN. BMC Oral Health 2022; 22(1):581.
Study data dictionary [will provide after main results have been accepted for publication]
Data set [will provide after main results have been accepted for publication]
Free Samples for Health (FreSH)
Study PI: Dr. Sandra Japuntich, Hennepin Healthcare
Brief Study Description
Cigarette smoking has profound negative effects on oral health. Smoking cessation decreases the incidence and progression of oral health problems. Most smokers attempt to quit, but the majority of quit attempts are unaided by smoking cessation medications and end in relapse. The American Dental Hygienists Association recommends that all oral health professionals Ask patients if they smoke, Advise smokers to quit, and Refer smokers to national quitlines for counseling (Ask-Advise-Refer; AAR). AAR connects patients directly to counseling but not to medication, which can double cessation rates independent of counseling. Indeed, few dentists prescribe smoking cessation medications. Failure to connect smokers to medication is a critical missed opportunity to prevent disease and save lives. Nicotine Replacement Therapy sampling (NRTS) refers to providing all smokers, regardless of their current interest in quitting, with free samples of over-the-counter NRT products and brief use instructions. NRTS has been shown to increase quit attempts, smoking cessation self-efficacy, and positive attitudes toward NRT. Dental settings are an ideal fit for NRTS because NRTS could easily be combined with AAR and providing samples of oral care products is routine and universal in dental care settings. The proposed UG3/UH3 project will test the effectiveness of NRTS in dental practices. In the 2-year Clinical Trial Planning Phase (UG3), we will complete all required milestones to establish feasibility and acceptability of study protocols and prepare for the 3-year Clinical Trial Implementation Phase (UH3). UG3 activities will include stakeholder interviews to evaluate initial acceptability and feasibility of proposed study interventions and procedures, pilot testing, protocol refinement, and recruitment of practices for the UH3 trial. In the UH3 trial, we propose to conduct a group randomized, hybrid type 1 implementation-effectiveness trial comparing AAR + NRTS (NRTS) to enhanced usual care (ET; AAR + electric toothbrush) in dental practices (N = 50 practices; N = 1200 patients) recruited from the Northeast and Midwest Regions of the National Dental Practice-Based Research Network. Study interventions will be delivered within the practices by trained practice staff. Our central hypothesis is that NRTS will produce greater abstinence rates than ET. Our primary outcome will be biologically verified, 7-day point prevalence abstinence at 6-months post-enrollment. We also predict that compared to ET, NRTS will increase rates of quit attempts, reduce smoking heaviness, and increase NRT utilization. We will conduct a multi-stakeholder process evaluation of the feasibility and acceptability of the NRTS intervention and a cost-effectiveness analysis to aid future implementation efforts. Overall, we expect that, as a result of this project, we will establish the feasibility, acceptability, and effectiveness of NRTS in dental practices and determine that NRTS has high potential for translation to clinical practice.
Key study publications:
Fang P, Adkins-Hempel M, Lischka T, Basile S, Rindal DB, Carpenter MJ, Kopycka-Kedzierawski DT, Dahne J, Helseth SA, Levy DE, Truong A, Leo MC, Funkhouser K, Louis DR, Japuntich SJ, National Dental PBRN Collaborative Group. A National Dental Practice-Based Research Network phase II, cluster-randomized clinical trial assessing nicotine replacement therapy sampling in dental settings: study protocol for the Free Samples for Health (FreSH) study. BMC Oral Health 2024; 24(1): 1007.
Japuntich SJ, Dunbar MS, Predmore Z, Bloom EL, Fang P, Basile S, Rindal DB, Waiwaiole LA, Carpenter MJ, Kopycka-Kedzierawski DT, Dahne J, Lischka TR, Richardson P, National Dental PBRN Collaborative Group. Dental staff and patient attitudes about nicotine replacement therapy samples in dental care: A National Dental Practice Based Research Network study. Community Dentistry and Oral Epidemiology 2024; 52(4):440-451.
Study data dictionary [will provide after main results have been accepted for publication]
Data set [will provide after main results have been accepted for publication]
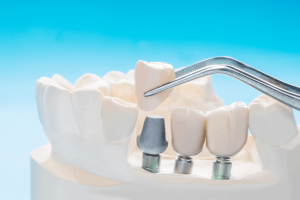
Dental Implant Restoration Registry (DIRR)
Study PI: Dr. Joana Cunha-Cruz, University of Alabama at Birmingham
Brief Study Description
There is a substantial body of literature to support that biological and prosthetic complications occur which may interfere with the health of the peri-implant tissues, the function and esthetics of the implant restoration. Peri-implant diseases are classified into peri-implant mucositis, inflammation restricted to the peri-implant mucosa, and peri-implantitis, characterized by peri-implant bone loss. The limitations of the current body of literature of biologic and prosthetic complications are based on many small studies and in large part conducted in an academic and specialty setting. We propose to create an implant registry within the National Dental Practice-Based Research Network (NDPBRN) that will record the setting and implant therapy, the implants used, the prosthetic therapy provided and the rate of complications. The registry will create an opportunity for subsequent, additional targeted studies on specific complications available from the registry data and will lead to diagnosis driven therapy strategies. The target enrollment is a total of 2000 implants with prosthesis across the whole network. The one year UG3 Phase will be used to create a strategy to be able to meet the recruitment and enrollment objectives and to develop the protocol for data collection to facilitate the data gathering of the practitioners for the subjects they enroll. The data collection model we propose will be designed to be validated, concise, and easy to use for practitioners. We will develop a web based decision tree that will guide the practitioner through the data collection. The UH3 phase will recruit practitioners with representation of all 6 regions of the network that will enroll subjects with 2000 implants. Data collection will be detailed and comprehensive and will include surgical, prosthetic, and biologic aspects of implant therapy and radiographs for bone level assessments for a period of 3 years. The data will present clinically meaningful information about the prevalence of the various implant therapies, the incidence of prosthetic and biologic implant complications, risk factors for implant complications and evidence-based implant therapy strategies in every dental practices. We expect that the results from this study will significantly impact the clinical practice of implant dentistry and the quality of care provided for the patients.
Key study publication:
Cunha-Cruz J, Barton D, Cochran D, Crawford P, Fahimipour F, Funkhouser EM, Geurs NC, Gilbert GH, Johnson JD, Kaur M, Smith N, Startley SJ, Stewart K, Waiwaiole L, National Dental PBRN Collaborative Group. The National Dental Practice-Based Research Network Dental Implant Restoration Registry to evaluate dental implant outcomes in community practice settings: protocol for a prospective observational study. JMIR Research Protocols 2026; 15:e82795.
Forms completed by practitioners
Study data dictionary [will provide after main results have been accepted for publication]
Data set [will provide after main results have been accepted for publication]
Periodontal Adjunctive Antibiotics Study (PAAS)
Study PI: Dr. Georgios Kotsakis
Brief Study Description
The objective of this study is to assess the effectiveness of adjunctive Amoxicillin / Metronidazole combination antibiotics to non-surgical periodontal therapy in clinical practices within the National Dental PBRN by conducting the largest randomized clinical trial (RCT) of adjunctive antibiotics. Further, within this PBRN study current decision-making factors for adjunctive antibiotic prescription will be surveyed to assess the state of affairs in clinical practice. Importantly, leveraging the well-powered RCT dataset, high responders to adjunctive antibiotic treatment will be identified and the predictive validity of decision-making factors currently employed by clinicians will be assessed to develop clear indications for prescription. Collectively, results of adjunctive antibiotic use at present are ambiguous because indications are based on empirical information without evidence-based guidelines, which may lead to antibiotic misuse and lack of efficacy. The present pragmatic well-powered RCT was designed to enable the development of evidence-based guidelines for periodontal adjunctive antibiotic use and promote antibiotic stewardship in dental practice.
Key study publications: [pending]
Study forms completed by practitioners
Study forms completed by patients
Study data dictionary [will provide after main results have been accepted for publication]
Data set [will provide after main results have been accepted for publication]
Conducted between 2012-2020
Predominately funded by NIH grant U19-DE-022516
Studies for which data collection has ended (n=17)
Study PI: Dr. Greg Huang, University of Washington
Brief Study Description
Almost all research on AOB treatment and stability is from retrospective case series. Therefore, this study had tremendous potential to provide practitioners with stronger evidence about AOB treatment outcomes and stability for adults. It also provided information about retention outcomes. Additionally, the gathering of patient-reported data about the decision to pursue a specific treatment option and patient satisfaction after treatment was extremely valuable.
This was a prospective, observational 3.5 year cohort study of approximately 840 adult patients in active orthodontic treatment for AOB who expected to have treatment completed within 24 months of enrollment into the study from approximately 210 National Dental PBRN orthodontists or dentists who routinely performed orthodontic treatment.
Objectives:
The primary objective was to estimate the proportion of patients 1) treated successfully (determined at the end of active treatment), and 2) whose treatment was stable (determined at one year post-active treatment).
The primary outcome measure to determine success of treatment was overbite at the end of treatment, and the primary measure to determine the stability of treatment ascertained one year after removal of orthodontic appliances was the overbite measurement.
Key study publications:
Greenlee GM, Collins JL, LeRoux B, Dolce C, Jolley C, Kau CH, Shin K, Vermette M, National Dental PBRN Collaborative Group, Huang GJ. Treatment outcomes and short-term stability in adult anterior open bite patients treated with or without extractions: a National Dental PBRN study. Angle Orthodontist 2025; 95(2):149-156.
Greenlee GM, Lewandowski L, Funkhouser E, Dolce C, Jolley C, Kau CH, Shin K, Allareddy V, Vermette M, National Dental PBRN Collaborative Group, Huang GJ. Treatment acceptance in adult anterior open bite patients: a National Dental PBRN study. American Journal of Orthodontics and Dentofacial Orthopedics 2024; 166(4):363-374.
Gu D, Leroux B, Finkleman S, Todoki L, Greenlee G, Allareddy V, Jolley C, Vermette M, Shin K, Kau CH, de Jesus-Vina J, Dolce C, National Dental PBRN Collaborative Group; Huang G. Anterior openbite malocclusion in adults: treatment stability and patient satisfaction in National Dental Practice-Based Research Network patients. Angle Orthodontist 2022; 92(1):27-35.
Todoki LS, Finkleman SA, Choi KW, Ko HC, Wang HF, Shapiro PA, Khosravi R, Baltuck C, Funkhouser E, Greenlee GM, Allareddy V, Dolce C, Kau CH, Shin K, Jolley C, Vermette M, Huang G, National Dental Practice-Based Research Network Collaborative Group. The National Dental Practice-Based Research Network Adult Anterior Open Bite Study: Treatment success. American Journal of Orthodontics and Dentofacial Orthopedics 2020; 158(6)e137-e150.
Finkleman SA, Todoki LS, Funkhouser E, Greenlee GM, Choi KW, Ko HC, Wang HF, Shapiro PA, Khosravi R, Baltuck C, Allareddy V, Dolce C, Kau CH, Shin K, de Jesus-Vinas J, Vermette M, Jolley C, National Dental Practice-Based Research Network Collaborative Group and Huang GJ. The National Dental Practice-Based Research Network Adult Anterior Open Bite Study: patient satisfaction with treatment. American Journal of Orthodontics and Dentofacial Orthopedics 2020; 158(6):e121-e136.
Huang G, Baltuck C, Funkhouser E, Wang HF, Todoki L, Finkleman S, Shapiro P, Khosravi R, Ko HC, Greenlee G, DeJesus-Vinas J, Vermette M, Larson M, Dolce C, Kau CH, Hamick D, National Dental PBRN Collaborative Group. The National Dental Practice-Based Research Network adult anterior openbite study: treatment recommendations and their association with patient and practitioner characteristics. American Journal of Orthodontics & Dentofacial Orthopedics 2019; 156(3):312-325.
Choi KW, Ko HC, Todoki LS, Finkleman SA, Khosravi R, Wang HF, Funkhouser E, Baltuck C, Raj V, Allareddy V, Matunas JC, Vermette ME, Harrell WE Jr, Coro JC, Greenlee GM, Huang GJ, National Dental PBRN Collaborative Group. The National Dental PBRN adult anterior openbite study: a description of the practitioners and patients. Angle Orthodontist 2018; 88(6): 675-683.
Data set 1 (Data set link is best downloaded through Internet Explorer)
Data set 2 (Data set link is best downloaded through Internet Explorer)
Data set 3 (Data set link is best downloaded through Internet Explorer)
Data set 4 (Data set link is best downloaded through Internet Explorer)
Data set 5 (Data set link is best downloaded through Internet Explorer)
Data set 6 (Data set link is best downloaded through Internet Explorer)
Data set 7 (Data set link is best downloaded through Internet Explorer)
Data set 8 (Data set link is best downloaded through Internet Explorer)
Data set 9 (Data set link is best downloaded through Internet Explorer)
Listed below were the forms for the study:
Practitioner characteristics form
Practitioner’s enrollment visit form
Patient’s enrollment visit form
Practitioner’s end of active treatment form
Patient’s end of active treatment form
Practitioner’s retainer use form
Study PI: Dr. Tom Hilton, Oregon Health Sciences University
Brief Study Description
This was a prospective, observational 4-year cohort study of both symptomatic and asymptomatic cracked teeth in 3,000 patients of ages 19-85 from 150-300 National Dental PBRN practices. Subjects received patient-, tooth- and crack-level assessments of a cracked tooth at baseline and follow-up visits over the subsequent four years.
Objectives:
The primary objective of the study was to identify patient-, tooth-, and crack- level characteristics associated with initial tooth symptom status, and to determine, over a four-year follow-up period, the associations of these multi-level factors with changes (tooth “failure”) that occured in an initially symptomatic or asymptomatic cracked tooth. Changes in the study tooth over time—outcomes that define the development of tooth “failure”– included crack progression, sign/symptom development, need for restorative dentistry, endodontic therapy or tooth extraction, development of periradicular lucency and loss of pulp vitality.
Many teeth required treatment over the course of the study period. Therefore, secondary objectives of the study were to:
- Identify multi-level (practice-, practitioner-, patient-, tooth-, and crack- level) factors associated with treatment recommendations for asymptomatic and symptomatic teeth provided by practitioners across the US;
- Identify associations between crack characteristics and time-to-treatment rendered during the four-year follow-up period;
- Determine, among treated cracked teeth, associations between the external and internal crack characteristics, which included externally detectable characteristics and internal characteristics that are observed during invasive treatment of the tooth.
- Evaluate outcomes of various treatments rendered on cracked teeth by determining associations between treatment rendered and time to tooth failure after treatment has been rendered on cracked teeth during the four-year follow-up period. These tooth outcomes include crack progression, sign/symptom development, and further recommended treatment of the tooth, development of periradicular lucency and loss of pulp vitality.
Key study publications:
Ferracane JL, Hilton TH, Funkhouser E, National Dental PBRN Collaborative Group. Lessons learned from the Cracked Tooth Registry –a three-year clinical study in the Nation’s Network. Journal of the American Dental Association 2023; 154(3):235-244.
Funkhouser E, Ferracane JL, Hilton TH, Gordan VV, Gilbert GH, Mungia R, Burton V, Meyerowitz C, Kopycka-Kedzierawski DT, National Dental PBRN Collaborative Group. Onset and resolution of pain among treated and untreated posterior teeth with a visible crack: three-year findings from The National Dental Practice-Based Research Network. Journal of Dentistry 2022; 119:104078. Click here to see two supplemental tables about the final status of teeth in the study and the timing and types of surgical procedures performed.
Ferracane JL, Hilton TJ, Funkhouser E, Gordan VV, Gilbert GH, Mungia R, Burton V, Meyerowitz C, Kopycka-Kedzierawski DT, National Dental PBRN Collaborative Group. Outcomes of treatment and monitoring of posterior teeth with cracks: three-year results from the National Dental Practice-Based Research Network. Clinical Oral Investigations 2022; 26(3):2453-2463.
Hilton TJ, Funkhouser E, Ferracane JL, Gilbert GH, Gordan VV, Kopycka-Kedzierawski DT, Meyerowitz C, Mungia R, Burton V for the National Dental PBRN Collaborative Group. Baseline characteristics as 3-year predictors of tooth fracture and crack progression: Findings from the National Dental Practice-Based Research Network. Journal of the American Dental Association 2021; 152(2):146-156.
Hilton TJ, Funkhouser E, Ferracane JL, Gilbert GH, Gordan VV, Bennett S, Bone J, Richardson PA, Malmstrom H, National Dental PBRN Collaborative Group. Symptom changes and crack progression in untreated cracked teeth: One-year findings from the National Dental Practice-Based Research Network. Journal of Dentistry 2020; 93:103269.
Hilton TJ, Funkhouser E, Ferracane JL, Schultz-Robins M, Gordan VV, Bramblett BJ, Snead RM, Manning W, Remakel JR, National Dental PBRN Collaborative Group. Recommended treatment of cracked teeth: results from the National Dental PBRN. Journal of Prosthetic Dentistry 2020; 123(1): 71-78.
Ferracane JL, Funkhouser E, Hilton TJ, Gordan VV, Graves C, Giese KA, SHea W, Pihlstrom DJ, Gilbert GH, National Dental PBRN Collaborative Group. Observable characteristics coincident with internal cracks in teeth: findings from the National Dental Practice-Based Research Network. Journal of the American Dental Association 2018; 149(10):885-892.
Hilton TJ, Funkhouser E, Ferracane JL, Gordan VV, Huff KD, Barna J, Mungia R, Marker T, Gilbert GH, National Dental PBRN Collaborative Group. Associations of types of pain with crack-level, tooth-level and patient-level characteristics in posterior teeth with visible cracks: findings from the National Dental Practice-Based Research Network. Journal of Dentistry 2018; 70(1): 67-73.
Hilton TJ, Funkhouser E, Ferracane JL, Gilbert GH, Baltuck C, Benjamin PL, Louis D, Mungia R, Meyerowitz, National Dental PBRN Collaborative Group. Correlation between symptoms and external cracked tooth characteristics: findings from the National Dental Practice-Based Research Network. Journal of the American Dental Association 2017; 148(4):246-256.
Data set 1 (Data set link is best downloaded through Internet Explorer)
Data set 2 (Data set link is best downloaded through Internet Explorer)
Data set 3 (Data set link is best downloaded through Internet Explorer)
Abstracts of study results presented at the 2016 American Association for Dental Research meeting.
This was an observational study examining the natural history of posterior cracked teeth, in which initial screening, patient enrollment, informed consent, initial data collection, and treatment (if indicated) were completed at baseline. Subsequent annual recalls are completed and follow-up data recorded. Treatment on a study tooth was always documented.
At the initial baseline visit, the following forms were used: patient characteristics, baseline: exam and treatment form, and reference worksheet.
For recall visits, the reference worksheet and appropriate (year 1, 2, 3) annual follow-up exam and treatment forms are completed.
For treatment accomplished other than at baseline or annual recalls, the treatment visit form was used.
If a patient will no longer participated in the study, a discontinuation form is filled out.
If a patient moved from the study practice, and was unwilling or unable to see a network dentist to continue data collection, a patient telephone interview guide and form was used to obtain information.
Appendix E for the subject retention plan
Study PI: Dr. Sonia Makhija, University of Alabama at Birmingham
Brief Study Description
The study examined the use of two diagnostic devices on dental practitioners’ identification and treatment of SOCLs. A total of 90 practitioners throughout the nation collected and recorded descriptive and treatment information for 40 SOCLs (one lesion/patient), 20 during the pre-intervention period and 20 during the intervention period. Practitioners were randomized into one of three arms: no diagnostic device, DIAGNOdent, and Spectra. They also completed diagnostic vignettes at the beginning and end of each study, as well as a post-study questionnaire.
Objectives:
The primary objective of the study was to quantify the difference in proportion of SOCLs treated operatively when a diagnostic device was used compared to when one was not used, and to quantify the difference in proportion of SOCLs treated operatively that extended into dentin when a diagnostic device is used compared to when one was not used.
The secondary objectives of the study were to:
- Identify the clinical characteristics of SOCLs that best predict caries that extend into dentin;
- Determine whether the principal factors used by participating practitioners in managing SOCLs change when a caries detecting device is employed; and
- Obtain practitioners’ assessments of the utility of the devices in their practices.
Key study publications:
Makhija SK, Bader JD, Shugars DA, Litaker MS, Nagarkar S, Gordan VV, Rindal DB, Pihlstrom DJ, Mungia R, Meyerowitz C, Gilbert GH, National Dental PBRN Collaborative Group. Influence of 2 caries-detecting devices on clinical decision making and lesion depth for suspicious occlusal lesions: a randomized trial from the National Dental Practice-Based Research Network. Journal of American Dental Association 2018; 149(4): 299-307.
Makhija SK, Robinson ME, Bader JD, Shugars DA, Litaker MS, Im HR, Rindal DB, Pihlstrom DJ, Meyerowitz C, Gordan VV, Buchberg M, Gilbert GH, National Dental PBRN Collaborative Group. Dentists’ decision strategies for suspicious occlusal caries lesions in a National Dental PBRN Study. Journal of Dentistry 2018; 69(2):83-87.
Makhija SK, Shugars DA, Gilbert GH, Litaker MS, Bader JD, Schaffer R, Gordan VV, Rindal DB, Pihlstrom DJ, Mungia R, Meyerowitz C, National Dental PBRN Collaborative Group. Surface characteristics and lesion status of suspicious occlusal carious lesions: findings from the National Dental Practice-Based Research Network. Journal of the American Dental Association 2017; 148(12):922-929.
Data set 1 (Data set link is best downloaded through Internet Explorer)
Data set 2 (Data set link is best downloaded through Internet Explorer)
Data set 3 (Data set link is best downloaded through Internet Explorer)
Data set 4 (Data set link is best downloaded through Internet Explorer)
Data set 5 (Data set link is best downloaded through Internet Explorer)
This study consisted of two phases: pre-intervention and intervention.
For the pre-intervention phase, the following forms were used: pre-study vignettes, consecutive eligible patient log, patient characteristics form, and dentist assessments form.
For the intervention phase, the following forms were used: consecutive eligible patient log, patient characteristics form, dentist assessments form for those assigned to a device and no device, and post-study vignettes for those assigned to the Spectra, DIAGNOdent, and no device.
Abstracts of study results presented at the 2016 and 2017 American Association for Dental Research.
Summary of study results for the pre-intervention and intervention phases.
Study PI: Dr. Michael McCracken, University of Alabama at Birmingham
Brief Study Description
This study examined patient, dentist, and laboratory factors associated with the fabrication of successful crowns. Each year, dentists must re-do thousands of crowns that are returned from the dental laboratory but are not clinically acceptable. It is not clear why some of these crowns are unsatisfactory. This clinical study that analyzed dentist and clinical variables to find predictors for crown success. Data from dental laboratories was collected in the clinical study to determine the prevalence of acceptable impressions, crown preparations and jaw relation records sent to labs for crown fabrication.
Key study publications:
Lawson NC, Litaker MS, Sowell E, Gordan VV, Mungia R, Ronzo KR, Lam BT, Gilbert GH, McCracken MS, National Dental PBRN Collaborative Group. Clinical acceptance of single-unit crowns and its association with impression and tissue displacement techniques: findings from the National Dental Practice-Based Research Network. Journal of Prosthetic Dentistry 2020; 123(5):701-709.
McCracken MS, Litaker MS, Thomson AES, Slootsky A, Gilbert GH, National Dental PBRN Collaborative Group. Laboratory technician assessment of the quality of single-unit crown preparations and impressions as predictors of clinical acceptability of crowns as determined by the treating dentist: findings from the National Dental Practice-Based Research Network. Journal of Prosthodontics 2020; 29(2):114-123.
Lawson NC, Litaker MS, Ferracane JL, Gordan VV, Atlas AM, Rios T, Gilbert GH, McCracken MS, National Dental PBRN Collaborative Group. Choice of cement for single-unit crowns: findings from the National Dental Practice-Based Research Network. Journal of the American Dental Association 2019; 150(6):522-530.
McCracken MS, Litaker MS, Gordan VV, Karr T, Sowell E, Gilbert GH, National Dental PBRN Collaborative Group. Remake rates for single-unit crowns in clinical practice: findings from the National Dental Practice-Based Research Network. Journal of Prosthodontics 2019; 28(2):122-130.
Data set 1 (Data set link is best downloaded through Internet Explorer)
Data set 2 (Data set link is best downloaded through Internet Explorer)
Data set 3 (Data set link is best downloaded through Internet Explorer)
Data set 4 (Data set link is best downloaded through Internet Explorer)
Data set 5 (Data set link is best downloaded through Internet Explorer)
The clinical study involved the following forms:
Enrollment/Baseline: consecutive eligible patient log; patient characteristics form; crown preparation form; and laboratory checklist
Final Study Visit: crown insertion form
The laboratory completed the laboratory questionnaire to evaluate technical aspects of the impression and preparation.
If a patient no longer participated in the study, a discontinuation form is completed.
Study PI: Dr. Michael McCracken, University of Alabama at Birmingham
Brief Study Description
This study examined patient, dentist, and laboratory factors associated with the fabrication of successful crowns. Each year, dentists must re-do thousands of crowns that are returned from the dental laboratory but are not clinically acceptable. It is not clear why some of these crowns are unsatisfactory. This was a questionnaire that documented current practices among clinicians making crowns, such as material choices and impression techniques.
Key study publications:
Minye HM, Gilbert GH, Litaker MS, Mungia R, Meyerowitz C, Louis D, Slootsky A, Gordan VV, McCracken MS, National Dental PBRN Collaborative Group. Preparation techniques used to make single-unit crowns: findings from the National Dental Practice-Based Research Network. Journal of Prosthodontics 2018; 27(9):813-820.
McCracken MS, Louis DR, Litaker MS, Minye HM, Oates T, Gordan VV, Marshall DG, Meyerowitz C, Gilbert GH, National Dental PBRN Collaborative Group. Impression techniques used for single-unit crowns: findings from the National Dental Practice-Based Research Network. Journal of Prosthodontics 2018; 27(8): 722-732.
McCracken MS, Litaker MS, George AJ, Durand S, Malekpour S, Marshall DG, Meyerowitz C, Carter L, Gordan VV, Gilbert GH, National Dental PBRN Collaborative Group. Impression evaluation and laboratory use for single-unit crowns: findings from the National Dental Practice-Based Research Network. Journal of the American Dental Association 2017; 148(11):788-796.
Makhija SK, Lawson NC, Gilbert GH, Litaker MS, McClelland J, Louis DR, Gordan VV, Pihlstrom DJ, Meyerowitz C, Mungia R, McCracken M, National Dental PBRN Collaborative Group. Dentist material selection for single-unit crowns: findings from the National Dental Practice-Based Research Network. Journal of Dentistry 2016; 55:40-47.
McCracken MS, Louis DR, Litaker MS, Minye HM, Mungia R, Gordan VV, Marshall D, Gilbert GH, National Dental PBRN Collaborative Group. Treatment recommendations for single-unit crowns: findings from the National Dental Practice-Based Research Network. Journal of the American Dental Association 2016; 147(11):882-890.
Data set (Data set link is best downloaded through Internet Explorer)
Stage 1 Full questionnaire
Supplemental table A1 includes the distribution of respondents’ likelihood of recommending a single-unit crown based on four scenarios in Figure 1 of the main manuscript, by dentist and practice characteristics.
Appendix Table 1A included the distribution of the responses to accept or reject an impression
Abstracts of study results presented at the American Association for Dental Research
Network enrollment questionnaire
Appendix Table 3 included the association of practitioner and practice characteristics with agreement on the practitioners’ top three treatment recommendations
Study PI: Dr. Gregg Gilbert, University of Alabama at Birmingham
Brief Study Description
The study assessed isolation techniques used when performing root canal treatment among dentists in the network. A questionnaire was administered to eligible dentists in the network. The questionnaire assessed dentists’ use of various isolation techniques when performing root canal treatment; identified factors associated with use (or non-use) of rubber dams when performing root canal treatment (RCT); and identifed factors associated with rubber dam use during RCT.
Objectives:
The primary objective of the study was:
- To quantify the self-reported use or non-use of rubber dams when performing RCT.
The secondary objective was:
- To identify factors associated with use or non-use of rubber dams for RCT.
Key study publications:
Funkhouser E, Vellala K, Baltuck C, Cacciato R, Durand E, McEdward D, Sowell E, Theisen SE, Gilbert GH, National Dental PBRN Collaborative Group. Survey methods used to optimize response rate in the National Dental Practice-Based Research Network. Evaluation and the Health Professions 2017; 40(3):332-358.2-358.
Eleazer PD, Gilbert GH, Funkhouser E, Reams GJ, Law AS, Benjamin PL, National Dental PBRN Collaborative Group. Techniques and materials used by general dentists during endodontic treatment procedures: findings from the National Dental Practice-Based Research Network. Journal of the American Dental Association 2016; 147(1):19-27.
Gilbert GH, Riley JL III, Eleazer PD, Benjamin PL, Funkhouser E, National Dental PBRN Collaborative Group. Discordance between presumed standard of care and actual clinical practice: the example rubber dam use during root canal treatment in the National Dental Practice-Based Research Network. BMJ Open 2015; 5(12):e009779.
Lawson NC, Gilbert GH, Funkhouser E, Eleazer PD, Benjamin PL, Worley DC, National Dental PBRN Collaborative Group. General dentists’ use of isolation techniques during root canal treatment: from the National Dental Practice-Based Research Network. Journal of Endodontics 2015; 41(8):1219-1225.
Data set (Data set is best downloaded through Internet Explorer)
View the full questionnaire.
Supplemental tables 1-6 include the distribution of the characteristics of eligible practitioners and their association with participation in the study; practitioners by tooth type for which they do root canal treatment; type and frequency of isolation method used; practitioner/practice characteristics by rubber dam use; stratified by frequency whether they perform root canal treatment on molars; as associations with using a rubber dam all the time.
Supplemental tables A1-A2 include frequency distribution for each attitude question item and a multivariable logistic regression of dentists’ attitudes about rubber dam use and whether or not they use a rubber dam 90% of the time or more often.
Supplemental table 3A includes logistic regressions of practitioner characteristics associated with use of endodontic methods characterized as ‘inappropriate’ by the endodontist authors.
View a pdf version of the National Dental PBRN Enrollment Questionnaire.
Study PI: Dr. Thankam Thyvalikakath, Indiana University
Brief study description:
This study investigated the feasibility of electronic clinical data reuse for research purposes. It was a proof-of-concept retrospective cohort study on the utility of electronic dental records data to assess outcomes of posterior composite restorations (PCR) and tooth loss following root canal treatment (RCT) (regardless of whether the tooth received dental restorations following RCT or not). An important second goal of this study is to determine the extent to which electronic dental records data may support obtaining reliable study outcomes for National Dental PBRN studies.
Key study publications:
Thyvalikakath T, Siddiqui Z, Eckert G, LaPradd M, Duncan WD, Gordan VV, Rindal DB, Jurkovich M, Gilbert GH, National Dental PBRN Collaborative Group. Survival analysis of posterior composite restorations in National Dental PBRN general dentistry practices. Journal of Dentistry 2024; 141:104831.
Thyvalikakath T, LaPradd M, Siddiqui Z, Duncan WD, Eckert G, Medam JK, Rindal DB, Jurkovich M, Gilbert GH, National Dental PBRN Collaborative Group. Root canal treatment survival analysis in National Dental PBRN practices. Journal of Dental Research 2022; 101(11): 1328-1334.
Thyvalikakath TP, Duncan WD, Siddiqui Z, LaPradd M, Eckert G, Schleyer T, Rindal DB, Jurkovich M, Shea T, Gilbert GH, National Dental PBRN Collaborative Group. Leveraging electronic dental record data for clinical research in the National Dental PBRN practices. Applied Clinical Informatics 2020; 11(2):305-314.
Data set [this data set is too large to store on this web site. If you would like access, please email Gregg Gilbert at [email protected]]
As part of the recruitment process, practitioners were provided background information and a FAQ page.
View an Excel file of reason(s) for Posterior Composite Resin failures.
Study PI: Dr. Dorota Kopycka-Kedzierawski, University of Rochester
Brief Study Description
This was a prospective cohort study of patients with dentin hypersensitivity. The study population consisted of adult dental patients who had dentin hypersensitivity and the practitioners who provided treatment for this condition. Approximately 180 dentists across the nation enrolled 14 study patients, with an enrollment aim of 2,520 adult patients for the entire network.
Objectives:
The primary objective of the study was to gain a better understanding of the multiple treatments used to manage dentin hypersensitivity among US dental practitioners by characterizing methods of diagnosing dentin hypersensitivity in the practice setting, dentists’ selected treatment(s) of dentin hypersensitivity, and patient-reported pain outcomes over time.
The secondary objectives of the study were to explore patient-, practitioner-, practice-, and tooth-level characteristics that contributed to practitioners’ selected treatment(s) and approach(es) to care and to characterize patients’ satisfaction with the received treatment of dentin hypersensitivity.
Key study publications:
Kopycka-Kedzierawski DT, Cacciato R, Hennessey R, Meyerowitz C, Litaker MS, Heft MW, Johnson KS, Reyes SC, Johnson JD, Baltuck CT, Gilbert GH, National Dental PBRN Collaborative Group. Electronic and paper mode of data capture when assessing patient-reported outcomes in the National Dental Practice-Based Research Network. Journal of Investigative and Clinical Dentistry 2019; 10(4): e12427.
Heft MW, Litaker MS, Kopycka-Kedzierawski DT, Meyerowitz C, Chonowski S, Yardic RL, Gordan VV, Mungia R, Gilbert GH, National Dental PBRN Collaborative Group. Patient-centered dentinal hypersensitivity treatment outcomes: results from the National Dental PBRN. JDR Clinical & Translational Research 2018; 3(1):76-82.
Kopycka-Kedzierawski DT, Meyerowitz C , Litaker MS, Heft MW, Tasgaonkar N, Day MR, Porter-Williams A, Gordan VV, Yardic RL, Lawhorn TM, Gilbert GH, National Dental PBRN Collaborative Group. Management of dentin hypersensitivity by practitioners in the National Dental Practice-Based Research Network. Journal of the American Dental Association 2017; 148(10):728-736.
Kopycka-Kedzierawski DT, Meyerowitz C, Litaker MS, Chonowski S, Heft MW, Gordan VV, Yardic RL, Madden TE, Reyes SC, Gilbert GH, National Dental PBRN Collaborative Group. Management of dentin hypersensitivity by National Dental PBRN practitioners: results from a questionnaire administered prior to initiation of a clinical study on this topic. BMC Oral Health 2017; 17(1):41.
Data set 1(Data set link is best downloaded through Internet Explorer)
Data set 2 (Data set link is best downloaded through Internet Explorer)
Data set 3 (Data set link is best downloaded through Internet Explorer)
Data set 4 (Data set link is best downloaded through Internet Explorer)
Appendix Table 1 showing the association of practitioner and patient characteristics with agreement on the practitioners’ top three treatment recommendations.
Abstract of study results presented at the American and International Association for Dental Research meetings.
Region-specific study results for the baseline and follow-up phases.
The primary aims of this study were to ascertain practitioners’ preferred methods of diagnosing and treating dentin hypersensitivity by completing a practitioner online questionnaire upon study enrollment.
To characterize diagnosis and treatment of dentin hypersensitivity in the practice setting, the following forms were used at baseline:
–Patient eligibility checklist
–Patient pain assessment baseline (1st line of treatment)
Forms were used at 1 week, 4 weeks, and 8 weeks.
1 week
–Patient pain assessment (1st line of treatment);Patient pain assessment (2nd line of treatment);Patient pain assessment (3rd line of treatment)
4 weeks
–Patient pain assessment (1st line of treatment);Patient pain assessment (2nd line of treatment);Patient pain assessment (3rd line of treatment)
8 weeks
–Patient pain assessment (1st line of treatment);Patient pain assessment (2nd line of treatment);Patient pain assessment (3rd line of treatment)
Other forms used include the following:
–Symptomatic exam form (2nd line treatment)
–Symptomatic exam form (3rd line treatment)
-Patient pain assessment (2nd line treatment)
-Patient pain assessment (3rd line treatment)
Appendix Table 3 includes the association of practitioner and practice characteristics with agreement on the practitioners’ top three treatment recommendations
Study PI: Dr. Eric Schiffman, University of Minnesota
Brief Study Description:
Temporomandibular Disorders (TMD) are the second most commonly occurring musculoskeletal disorders after chronic back pain resulting in pain and disability. Diagnosis and treatment of TMD are within the purview of general dentistry (NIDCR, 2009) with most patients consulting a general dentist regarding their painful TMD. Within the context of the National Dental Practice-Based Research Network (Network), the goal of this observational prospective cohort study was to identify factors contributing to TMD treatment decisions and treatment adherence, as well as the overall effect of TMD treatment on pain intensity and jaw function measured at 1-, 3- and 6-month follow-ups. We recruited approximately 200 dentist practitioners from the six National Dental PBRN regions (Northeast, South Atlantic, South Central, Southwest, Midwest, Western). Each participating dentist contributed to a total patient enrollment of approximately 1980.
Objectives:
The primary objective of this study was to identify the factors that contribute to practitioners’ treatment decisions for patients with painful TMD.
The secondary objectives of this study were to:
- Identify factors that contribute to patients’ adherence to treatment, and
- Describe observed changes from baseline at 1-, 3- and 6-month follow-up in pain intensity and jaw function associated with treatments.
The primary outcome measure of this study was the practitioners’ treatment decisions for painful TMD patients. The secondary outcome measures for this study were patient adherence, and pain intensity and jaw function measures. Numerous potential confounders and predictors were assessed for their associations with the treatment decisions, patient adherence, and changes in pain and function.
Key study publications:
Riley JL 3rd, Rindal DB, Velly AM, Anderson GC, Johnson KS, Gilbert GH, Schiffman ES, National Dental PBRN Collaborative Group. Practitioner/practice- and patient-based factors contributing to dental practitioners’ treatment recommendations for patients with pain-related TMDs: findings from the National Dental PBRN. Journal of Oral & Facial Pain & Headache 2023; 37(3):195-206.
Velly AM, Anderson GC, Look JO, Riley JL III, Rindal DB, Johnson K, Wang Q, Fricton J, Huff K, Ohrbach R, Gilbert GH, Schiffman E, National Dental PBRN Collaborative Group. Management of painful temporomandibular disorders: methods and overview of the National Dental Practice-Based Research Network prospective cohort study. Journal of the American Dental Association 2022; 152(2):144-157.
Study data dictionary and contents
Prior to beginning the study, doctors completed a doctor demographics form. At baseline, the patient completed a demographic form, contact form and a baseline questionnaire. The doctor completed a doctor initial questionnaire.
The patient completed follow-up questionnaires at 1-month, 3-months and 6-months. The doctor also completed a follow-up questionnaire at 6-months.
Study PI: Dr. Jeffrey Fellows, Kaiser Permanente Center for Health Research
Brief Study Description:
Severe post-operative pain following root canal therapy (RCT) occurs in about 20% of patients. The presence of persistent pain following RCT is about 10%, and initial evidence suggests that half of these patients experiencing persistent pain have a non-odontogenic etiology for this pain. Applying odontogenic strategies to treat non-odontogenic pain may increase incidence and duration of chronic oral pain. The overarching goal of this prospective observational cohort study was to investigate risk factors for severe pain following RCT, the prevalence and impact of persistent pain following RCT, and the impact of severe and persistent pain on health-related quality of life. Patient and treatment-related data was collected before and after RCT completion. Follow-up data was collected 1 week, 6 months, and 12 months following RCT completion. Approximately 150 practitioners from six National Dental PBRN regions enrolled approximately 1,650 adult patients.
Key study publications:
Liu LJ, Ordinola-Zapata R, Noblett WC, Funkhouser E, Law AS, Nixdorf DR, Lam E, Mungia R, Gilbert GH, National Dental PBRN Collaborative Group. Clinical and psychosocial predisposing factors associated with anesthesia failure during non-surgical root canal treatment: a National Dental PBRN study. Under review.
Law AS, Nguyen QC, Funkhouser E, Mungia R, Nixdorf DR, Lam EWN, Gilbert GH, National Dental PBRN Collaborative Group. Antibiotic prescribing associated with non-surgical root canal treatment: findings from the National Dental PBRN. Under review.
Allareddy V, Law AS, Cunha-Cruz J, National Dental PBRN Collaborative Group, Gilbert GH. Collaboration between the National Dental Practice-Based Research Network and the American Association of Endodontists: impact on the endodontic literature. Journal of the American Dental Association 2026; accepted for publication.
Mungia R, Law AS, Funkhouser E, Law AS, Nixdorf DR, Lam EWN, Gilbert GH, National Dental PBRN Collaborative Group. Opioid prescribing following non-surgical root canal therapy: findings from the National Dental Practice-Based Research Network. Journal of the American Dental Association 2026; accepted for publication.
Law AS, Berg R, Funkhouser E, Mungia R, Nixdorf DR, Gilbert GH, National Dental PBRN Collaborative Group. Factors associated with dental dam use during non-surgical root canal treatment: a National Dental PBRN study. Journal of Dentistry 2026; 164:106258.
Mungia R, Funkhouser E, Law AS, Nixdorf DR, Fellows JL, Gilbert GH, National Dental PBRN Collaborative Group. Occurrence and predictors of severe pain one week after root canal treatment: the National Dental PBRN PREDICT Endodontic Study. Journal of Dentistry 2026; 164:106232.
Mungia R, Funkhouser E, Law AS, Nixdorf DR, Lindquist KA, Caprio DS, Fellows JL, Gilbert GH. Prevalence and factors associated with severe pre-operative pain among patients presenting for root canal therapy in the National Dental PBRN PREDICT Endodontic Study. Journal of Dentistry 2025; 163:106147.
Law A, Nagarkar S, Funkhouser E, Mungia R, Nixdorf DR, Lam EWN, Roda RS, Gilbert GH. Factors affecting root canal treatment case difficulty, practitioner rating of difficulty, and treatment complications among general dentists and endodontists: a prospective cohort study from the National Dental PBRN PREDICT Project. International Endodontic Journal 2025; 58(12):1862-1871.
Nosrat A, Funkhouser E, Law A, Abusteit O, Mungia R, Nixdorf DR, Lam EWN, Gilbert GH. Differences in clinical approaches of endodontists and general dentists when performing non-surgical root canal treatment: a prospective cohort study from the National Dental PBRN PREDICT project. International Endodontic Journal 2025; 58(9):1408-1419.
Mungia R, Funkhouser E, Law AS, Nixdorf DR, Ruben RL, Gordan VV, Fellows JL, Gilbert GH. Characteristics of teeth and patients receiving root canal treatment in National Dental PBRN practices: comparison between endodontist and general dentist practices. Journal of Dentistry 2025; 157: 105723.
Lam EWN, Law AS, Nguyen RHN, Basile SM, Austah O, Gilbert GH, Lindauer PA, Romano MJ, Nixdorf DR, Fellows JL, National Dental Practice-based Research Network Collaborative Group. Inter-examiner agreement in the radiologic identification of apical periodontitis/rarefying osteitis in the National Dental PBRN PREDICT endodontic study. Journal of Endodontics 2021; 47(10):1575-1582.
At the baseline enrollment visit, patients completed tablet-based enrollment, contact information, and two surveys (before and after treatment) at the baseline enrollment visit.
Patient-reported follow-up data were collected by web-based or phone survey at 1 week, 6 months, and 12 months following the RCT completion visit date.
Practitioners completed web-based weekly recruitment logs during the recruitment period, a before treatment survey at the enrollment visit, an after RCT completion survey on the obturation date (some patients required multiple visits), and uploaded pre- and post-RCT radiographs to a study site.
Practitioners completed a 12-month survey and radiograph upload during a patient recal visit approximately one year after the RCT completion visit.
Study PI: Dr. Peter Lockhart, Charlotte Medical Center
Brief Study Description
Since the advent of antibiotics in the mid-1940s, and in particular with the first formal recommendations for antibiotic prophylaxis (AP) by the American Heart Association (AHA) in 1955, there has been a significant proliferation of the use of secondary AP in dental practice. However, there has been increasing controversy about the widespread use of antibiotics for some prophylactic, as well as therapeutic dental purposes, primarily due to concerns about antibiotic resistant bacteria and adverse drug reactions, weak evidence to support the practice of AP, and the costs and inconvenience associated with the use of AP. Consequently, this study aimed to identify critical conceptual and standardization gaps in the practice and implementation of AP for patient populations felt to be at increased risk to develop infective endocarditis (IE) and/or prosthetic joint infections (PJI) prior to dental procedures. By surveying approximately 2,500 members of the National Dental Practice-Based Research Network, the survey revealed some of the common tendencies and practices regarding AP by practitioners across the United States.
Key study publications:
Lockhart PB, Thornhill MH, Zhao J, Baddour LM, Davis, J, McKnight PE, Gilbert GH, Mungia R, Mougeot J-L, National Dental PBRN Collaborative Group. Prophylactic antibiotic prescribing in dental practice – findings from a National Dental Practice-Based Research Network questionnaire. Journal of the American Dental Association 2020; 151(10):770-781.
Mougeot J-L, Davis JM, Zhao J, Sullivan KA, Thornhill MH, McKnight PE, Stephens C, Lockhart PB, National Dental PBRN Collaborative Group. Methodology for the development of a National Dental Practice-Based Research Network survey on dentist’s beliefs and behaviors concerning antibiotic prophylaxis. Oral Surgery Oral Medicine Oral Pathology Oral Radiology 2020; 130(2):e29-e37.
Participants completed a questionnaire about their AP use.
Participating dentists also completed the network’s Enrollment Questionnaire.
Study PI: Dr. Jamie Studts, University of Kentucky
Brief Study Description
Using a single-arm trial design, this study examined the feasibility and acceptability of evaluating “QuitAdvisorDDS”, a clinical decision support software application designed to facilitate implementation of evidence-based tobacco treatment interventions into the dental setting. The study examined the impact of the QuitAdvisorDDS tool on patient outcomes related to tobacco use and cessation attempts as well as provider knowledge, attitudes, and practices regarding tobacco treatment. Practitioner (dentists and hygienists) completed surveys at baseline and follow-up, while patients completed surveys at baseline and 1-month follow-up. An embedded substudy also evaluated the feasibility and acceptability of collecting biospecimens (saliva) to serve as biochemical verification of smoking status.
Key study publication:
Stoops WW, Johnson MF, Strickland JC, Knudsen HK, Gilbert GH, Massingale SD, Ray MN, Studts CR, Atchley L, Reynolds G, Studts JL, National Dental PBRN Collaborative Group. Feasibility of collecting saliva for biological verification of tobacco use status in dental practices and patients’ homes: results from the National Dental PBRN. Community Dental Health 2019; 36(3):187-189.
This study received primary funding by R44-DE-021327. Consequently, the responsibility for public access to data from this study lies with that grant.
Study PI: Dr. Julia Melkers, Georgia Technical University
Brief Study Description
This study will characterize and examine the structure, content, and pathways of clinical information in the dental information ecosystem. It will also give attention to disruptive events that impact knowledge and information diffusion through a focus on alternative nicotine products (ANPs). The study will address the clinical information-seeking networks (both formal and informal) of dentists and hygienists. This is a multi-methodological 39-month study that will be conducted in the National Dental Practice-Based Research Network (National Dental PBRN). The study will involve one round of survey implementation, on-going bibliometric data collection and web scraping, as well as one round of feedback interviews via telephone.
Key study publications:
Isett KR, Doshi AM, Rosenblum S, Eller W, Hicks D, Melkers J, National Dental PBRN Collaborative Group. Temporal search persistence, certainty, and source preference in dentistry: results from the National Dental PBRN. PLOS One 2022; 17(5):e0264913.
Burgette JM, Isett KR, Rosenblum S, Doshi A, Melkers J for the National Dental PBRN Collaborative Group. Association between predoctoral evidence-based practice training and later use of peer-reviewed journals: National Dental PBRN. Journal of Dental Education 2021; 85(6): 812-820
Rosenblum S, Isett KR, Melkers J, Funkhouser E, Hicks D, Gilbert GH, Melkers MJ, McEdward D, Buchberg-Trejo M, National Dental PBRN Collaborative Group. The association between professional stratification and use of online sources: evidence from the National Dental Practice-Based Research Network. Journal of Information Science 2021; 47(3):373-386.
Hicks D, Melkers M, Barna J, Isett KR, Gilbert GH. Comparison of the accuracy of CBCT effective radiation dose information in peer-reviewed journals and dental media. General Dentistry 2019; 67(3):38-46.
Hicks D, Melkers J, Isett KR. A characterization of professional media and its links to research. Scientometrics 2019; 119(2):827-843.
Hicks D, Melkers M, Barna J, Isett KR, Gilbert GH. Comparison of the accuracy of CBCT effective radiation dose information in peer-reviewed journals and dental media. General Dentistry 2019; 67(3):38-46.
Melkers J, Hicks D, Isett KR, Kopycka-Kedzierawski DT, Gilbert GH, Rosenblum S, Burton V, Mungia R, Melkers MJ, Ford G, National Dental PBRN Collaborative Group. Preferences for peer-reviewed versus other publication sources: a survey of general dentists in the National Dental PBRN. Implementation Science 2019; 14(1):19.
Isett KR, Rosenblum S, Barna J, Hicks D, Fellows JL, Cochran D, Wiedner H, Gordan VV, Gilbert GH, Melkers J, National Dental PBRN Collaborative Group. Missed opportunities for detecting alternative nicotine product use in youth: data from the National Dental PBRN. Journal of Adolescent Health 2018; 63(5): 587-593.
Robinson-Garcia N, Trivedi R, Costas R, Isett K, Melkers J, Hicks D. The unbearable emptiness of tweeting – about journal articles. PlosOne 2017; 12(8):e0183551.
Melkers J, Hicks D, Rosenblum S, Isett K, Elliot J, Dental blogs, podcasts, and associated social media: descriptive mapping and analysis. Journal of Medical Internet Research 2017;19(7):e269.
Data set (Data set link is best downloaded through Internet Explorer)
Study PI: Dr. Jenna McCauley, Medical University of South Carolina
Brief Study Description
This study aimed to identify critical training gaps in dental implementation of opioid prescribing risk mitigation strategies. Dentists follow primary care physicians as the second leading prescriber of immediate release opioids. However, dentists typically have limited exposure to addiction training and may not be familiar with recommended opioid prescribing risk mitigation strategies. This study consisted of an online survey that documented current knowledge, training experiences, and practice behaviors related to acute dental pain management and opioid analgesic prescribing among member dentists. Data from the survey was paired with key practice-related enrollment data to identify aforementioned gaps in knowledge and directly inform the development of an educational intervention that provided dentists’ training in opioid misuse screening and implementation of risk mitigation strategies when prescribing opioids for acute pain management.
Key study publications:
McCauley JL, Nelson JD, Gilbert GH, Gordan VV, Durand SH, Mungia R, Meyerowitz C], Leite RS, Fillingim RB, Brady KT, National Dental PBRN Collaborative Group. Prescription drug abuse among patients in rural dental practices reported by members of the National Dental PBRN. Journal of Rural Health 2020; 36(2):145-151.
McCauley JL, Gilbert GH, Cochran D, Gordan VV, Leite RS, Fillingim RB, Brady KT, National Dental PBRN Collaborative Group. Prescription drug monitoring program use: National Dental PBRN results. JDR Clinical & Translational Research 2019; 4(2):178-186.
McCauley JL, Reyes S, Meyerowitz C, Gordan VV, Rindal DB, Gilbert GH, Leite RS, Fillingim RB, Brady KT, National Dental PBRN Collaborative Group. Training experiences regarding pain management, addiction, and drug diversion of dentists enrolled in the National Dental Practice Based Research Network. Substance Abuse 2019; 4:1-6.
McCauley JL, Leite RS, Gordan VV, Fillingim RB, Gilbert GH, Meyerowitz C, Cochran D, Rindal DB, Brady KT, National Dental PBRN Collaborative Group. Opioid prescribing and risk mitigation implementation in the management of acute pain: results from the National Dental PBRN. Journal of the American Dental Association 2018; 149(5): 353-362.
Data set (Data set link is best viewed in Internet Explorer)
Study PI: Dr. Maura Gillison, The Ohio State University
Brief Study Description
A target of 1,000 men and women aged 30-69 years were enrolled over a 6-month period, with up to 1,200 enrollments allowed to avoid cutting off enrollment in the middle of a business day. Thirty practice locations were recruited from the 6 National Dental PBRN regions (5 practice locations per region). Participating patients were recruited during routine clinical visits with participating National Dental PBRN practitioners. Each practitioner recruited 25-30 patients. Patients were provided with a tablet computer on which the study was explained, electronic consent was obtained, patient eligibility was assessed, an oral HPV risk factor survey was administered, and patient selection for oral rinse collection was determined. Based on survey responses, the top three deciles of risk (~300) and a random selection of 1 in 12 of those in the lower deciles (~59) were selected for oral rinse collection (~359 total). An oral rinse sample was obtained by means of a 30 second rinse and gargle with ScopeTM mouthwash (or saline), expectorated into a sterile specimen collection cup, sealed and stored at 4°C. Specimens were shipped by practice staff approximately weekly or twice a week to a central laboratory for human papillomavirus (HPV) detection. HPV results were communicated to the dental practitioner through the study’s secure web application. Patients with a high-risk oral HPV infection (anticipated to be ~25 individuals) were offered enrollment into a prospective study inclusive of a blood draw, an oral cancer examination, and a 6-month follow-up dental visit (window: 5-9 months) with a repeat oral rinse and an electronic oral cancer risk factor survey. Patients were compensated with a gift card for each major study procedure.
Objectives
The primary objective of this study were to estimate the proportion of the study population with an oral high-risk HPV infection.The secondary objectives of this study were to:
- Evaluate the feasibility and acceptability of baseline study procedures performed by participating patients and staff;
- Measure the distribution of demographic and behavioral characteristics associated with oral HPV infection;
- Determine compliance with and feasibility of procedures performed at a 6-month follow-up visit (window: 5-9 months), including blood draw, second oral rinse specimen collection, oral cancer screening examination, and completion of an oral cancer risk factor survey.
Key study publication:
Rindal DB, Gilbert GH, Carcelen C, Funkhouser E, Durand E, Uppgaard DA, Fellows JL, Ikeda J, Kerr AR, Brar B, Gordan VV, Agarwal S, Barnett P, Pickard RK, Gillison M, National Dental PBRN Collaborative Group. Feasibility and acceptance of oral HPV detection in the dental office: results from the National Dental PBRN. Journal of the American Dental Association 2019; 150(2):130-139.
Data set-patients (Data set link is best downloaded through Internet Explorer)
Data set-practitioners (Data set link is best downloaded through Internet Explorer)
- Electronic Study Summary, Part I Oral HPV Screening (Appendix A).
- Oral HPV Risk Factor survey (Appendix C)
- HNS providers completed a ROCS Oral Cancer Screening Examination Form
- Part II patients completed the Oral Cancer Risk Factor survey (Appendix J)
- ROCS Provider Survey (Appendix P) upon completion of all study procedures.
Study PI: Dr. Elizabeth Shenkman, University of Florida
Brief Study Description:
The dentist’s office may be an important setting for conducting multi-risk assessments (MRAs) for oral and physical health risks to increase opportunities for early assessment of and intervention for risk behaviors. This study characterized dental practitioners’ (dentists and hygienists), dental payers’, and patients’ attitudes about: (a) conducting/participating in MRAs during dental visits; and (b) providing/receiving follow-up counseling about and referrals for identified risks. An analysis was also conducted of the dentists’ and dental hygienists’ scope of practice documents to determine if there were any regulatory barriers for conducting MRAs, risk behavior counseling, and referrals.
Key study publications:
Guo Y, Woodard J, Zhang Y, Staras SAS, Gordan VV, Gilbert GH, McEdward DL, Shenkman EA, National Dental Practice-Based Research Network Collaborative Group. Patients’ comfort with and receipt of health risk assessments during routine dental visits: results from the South Atlantic region of the US National Dental Practice-Based Research Network. Community Dentistry and Oral Epidemiology 2023; 51(5):854-863.
Staras SAS, Guo Y, Gordan VV, Gilbert GH, McEdward DL, Manning D, Woodward J, Shenkman EA, National Dental Practice-Based Research Network Collaborative Group. Dental practitioners’ use of health risk assessments for a variety of health conditions: Results from the South Atlantic region of the National Dental Practice-Based Research Network. Journal of the American Dental Association 2021; 152(1):36-45.
Study data dictionary, data formats, and annotated Enrollment Questionnaire
Data sets –
Patients
Enrollment
Practices Provider
Practitioner
Tracking
See here for the data collection forms used in this study.
Participating dentists and hygienists also completed the network’s Enrollment Questionnaire.
Study PI: Dr. Walter Psoter, University of Rochester
Brief Study Description
Worldwide, there were an estimated 274,000 new cases and 127,000 deaths attributed to oral cancer (OC) (ICD-O C00-C06), and over 600,000 new cases of head and neck cancer (HNC) reported in 2008. Over 70% of U.S. dentists self-report performing oral cancer (screening) examination (OCE) on most of their patients over 40 years of age, although the completeness, quality, frequency and validity of these examinations are unknown. Regardless, 18% of adults (8% of Blacks and 7% of Latinos) aged 40 years and over are reported to have had an OC examination in the last year. Moreover, only 20% to 29% of adults reported ever having had an OCE. The overall goal of the project was to ascertain common practices related to oral cancer examinations by U.S. dentists and dental hygienists, by geographic region, demographics and practitioner and practice characteristics.
This was a National Dental Practice-Based Research Network (National Dental PBRN) survey study that consisted of 2 components: 1) a questionnaire survey (33 questions), and 2) sixteen standardized clinical case-vignette presentations with 6 specific process questions. National Dental PBRN general dentists and dental hygienists were invited to participate in the study to describe the details of the OCE, including who, what, when, where, and why, as well as the details involved with patient disposition of newly discovered “suspicious” for oral pre-malignant or malignant lesions.
Key study publications:
Psoter WJ, Kerr AR, Tomar SL, Psoter JA, Morse DE, Aguilar ML, Kligman KD, Minye HM, Burton VA. Diagnostic approach used by U.S. general dental practitioners following discovery of oral lesions suspicious for malignancy/premalignancy: findings from the National Dental Practice-Based Research Network. Quintessence International 2024; 55(8):652-659.
Kerr AR, Robinson ME, Meyerowitz C, Morse DE, Aguilar ML, Tomar SL, Guerrero L, Caprio D, Kaste LM, Makhija SK, Mungia R, Rasubala L, Psoter WJ, National Dental PBRN Collaborative Group. Cues used by dentists in the early detection of oral cancer and oral potentially malignant lesions: findings from the National Dental Practice-Based Research Network. Oral Surgery Oral Medicine Oral Pathology Oral Radiology 2020; S2212-4403(20)31011-7.
Psoter WJ, Morse DE, Kerr AR, Tomar SL, Aguilar ML, Harris DR, Stone LH, Makhija SK, Kaste LM, Strumwasser B, Pihlstrom DJ, Masterson EE, Meyerowitz C, National Dental PBRN Collaborative Group. Oral cancer examinations and lesion discovery as reported by U.S. general dentists: findings from the National Dental Practice-Based Research Network. Preventive Medicine 2019; 124:117-123.
Data set (Data set link is best downloaded through Internet Explorer)
This study consisted of 2 components:
1) a questionnaire survey
Conducted between 2005-2012
Predominately funded by NIH grants U01-DE-16746 and U01-DE-16747
Studies for which data collection has ended (n=23)
Study PI: Dr. Valeria Gordan, University of Florida
Brief Study Description
The purpose of this project was to identify methods that DPBRN dentists used to diagnose and treat caries lesions. The aims of this study were to: (a) quantify the percentages of DPBRN dentists who report using selected methods for caries diagnosis; (b) quantify the percentage of DPBRN dentists who report using a caries-risk assessment protocol of any variety; (c) quantify the percentages of DPBRN dentists who report intervening surgically at caries stages E1, E2, D1, D2, or D3. The aims were met by enrolling more than 500 DPBRN practitioner-investigators, each of whom completed a 10-page questionnaire about caries diagnosis and treatment assessment. Findings from this study were compared to treatment that was actually delivered as determined in DPBRN studies of primary and replacement restorations.
Key study publications:
Riley JL III, Rindal DB, Fellows JL, Gilbert GH, Ajmo CT, Amundson C, Anderson GA, Gordan VV for The DPBRN Collaborative Group. Preferences for caries prevention agents in adult patients: findings from The Dental PBRN. Community Dentistry and Oral Epidemiology 2010; 38(4): 360-370.
Riley III JL, Gordan VV, Rindal DB, Fellows JL, Williams OD, Ritchie LK Jr, Gilbert GH for The DPBRN Collaborative Group. General practitioners’ use of caries-preventive agents in adult patients versus pediatric patients: findings from The Dental Practice-Based Research Network. Journal of the American Dental Association 2010; 141(6): 679-687.
Gordan VV, Bader JD, Garvan CW, Richman JS, Qvist V, Fellows JL, Rindal DB, Gilbert GH for The DPBRN Collaborative Group. Restorative treatment thresholds for occlusal primary caries by dentists in The Dental PBRN. Journal of the American Dental Association 2010; 141(2):171-184.
Gordan VV, Garvan CW, Richman JS, Fellows JL, Rindal DB, Qvist V, Heft MW, Williams OD, Gilbert GH for The DPBRN Collaborative Group. How dentists diagnose and treat defective restorations: evidence from The Dental PBRN. Operative Dentistry 2009; 34(6): 664-673.
Data set (The data set is best downloaded through Internet Explorer)
Annotated version
View the questionnaire
View an article from the May 2012 issue of Dr. Biscupid
View an Excel file of reason(s) for Posterior Composite Resin failures.
Study PI: Dr. Andrei Barasch, University of Alabama at Birmingham
Brief Study Description
The incidence of diabetes mellitus has been increasing at epidemic proportions, making this chronic disease the most common medical condition in dental patients. Hyperglycemia has been identified as a potential risk factor for periodontal disease, disease infection, and poor response to treatment. Additionally, an estimated 4% of Americans are undiagnosed diabetics, and more than 80% of the diagnosed patients are not well-controlled. Early diagnosis and intervention have been shown to improve outcomes and reduce morbid medical complications in diabetic patients. Thus, identifying hyperglycemia in dental practice could lead to significant improvement in both the dental and medical outcomes.
This study investigated the prevalence of hyperglycemia in dental patients of DPBRN practitioner-investigators. The global aim of this study was to determine the feasibility of blood sugar testing and diabetes screening in dental practice. The specific aims of this study were to quantify the: 1) percentage of DPBRN patients who meet the American Diabetes Association screening criteria and describe the characteristics of these patients; and 2) acceptability of conducting blood sugar testing in the dental office and barriers to regular screening, as reported by DPBRN patients and practices.
*the terms ‘blood sugar’ , ‘blood glucose’, and ‘hyperglycemia’ are related and interchangeable in some contexts. DPBRN adopted the term ‘blood sugar’ for the title of this study to tailor its communication to a lay, non-dental, non-medical audience. This helps facilitate explaining the study to dental patients.
Key study publications:
Barasch A, Gilbert GH, Spurlock N, Funkhouser EM, Persson LL, Safford MM; DPBRN Collaborative Group. Random plasma glucose values measured in community dental practice: findings from The Dental Practice-Based Research Network. Clinical Oral Investigations 2013;17(5):1383-1388.
Barasch A, Safford MM, Palmore R, Gesko D, Gilbert GH for The DPBRN Collaborative Group. Random blood glucose testing in dental practice: a community-based feasibility study from The Dental Practice-Based Research Network. Journal of the American Dental Association2012; 143(3):262-269.
Annotated end of survey dentist form
Data set-dentist (The data set link is best downloaded through Internet Explorer)
Data set-patient (The data set link is best downloaded through Internet Explorer)
Data set-screening (The data set link is best downloaded through Internet Explorer)
This study used several data forms. The first one was the “Screening and Testing” form, which provided patient information and risk for diabetes mellitus.
If the patient qualified and agreed, this form also collected the glucose test result. Another form was a questionnaire answered by the patient.
Participants received a Physician Referral Letter and an information brochure about diabetes from the American Diabetes Association.
We also used a questionnaire completed by the practice’s dentist and staff ; it provided insights regarding the feasibility of and possible barriers to glucose testing in dental practice. Each Regional Coordinator also conducted an end-of-study interview of the participating practitioners. Finally, we used a “Consecutive Patient Log” and a “Master Participant List”.
Detailed report, overall and by region
Graphical presentation of study findings, overall and by region
Study PI: Dr. Andrei Barasch, University of Alabama at Birmingham
Brief Study Description
Osteonecrosis of the jaws (ONJ) is a potentially morbid and costly oral condition. In the recent past more than 200 cases of ONJ have been described in patients treated with bisphosphonates (BPs) for osseous cancer lesions or osteoporosis. The number of BP prescriptions has been steadily increasing, creating concerns about this potential side effect. The causes and risk factors for ONJ are not known. In this study we investigated these issues making use of the research infrastructure from the three dental practice-based research networks (PBRNs) funded by NIDCR.
The specific aims of this study were to test the hypotheses that: (1) BP treatment is a risk factor for ONJ; and (2) dental diseases, particularly periodontal disease and invasive dental procedures such as dental extractions are true risk factors for ONJ, or whether these procedures are a consequence of the necrotic disease process. This study quantified the impact that BP exposure had on the risk of developing ONJ, relative to comparable control patients, using a case-control study design. The risk factors studied included BPs, dental risk factors, and other factors, such as radiation and steroid therapy. All the patients with ONJ identified from the PBRNs were recruited for the study. Cases were identified by a dentist in the PBRN and were diagnosed by the dentist or a specialist as having ONJ with an onset between January 2005 and January 2007. Each case had three controls from the practice that identified the case. The dentist summarized the relevant dental treatment history and provided a dental disease diagnosis history from January 2000 until diagnosis of ONJ for cases, and until recruitment for controls. A professional centralized interviewer within each PBRN administered the same standardized questionnaire to cases and controls over the telephone.
Relevance to public health: This study was a unique and timely opportunity to investigate risk factors for ONJ, results from which may have a substantial impact on dental health and oral-related quality of life in an increasing number of patients.
Key study publications:
Barasch A, Cunha-Cruz J, Curro FA, DeRouen T, Gilbert GH, Hujoel P, Safford MM, Vena DA, Voinea-Griffin AE, Wu H for the CONDOR Collaborative Group. Dental risk factors for osteonecrosis of the jaws: a CONDOR case-control study. Clinical Oral Investigations 2013; 17(8): 1839-1845.
Barasch A, Cunha-Cruz J, Curro FA, Hujoel P, Sung AH, Vena D, Voinea-Griffin AE for the CONDOR Collaborative Group. Risk factors for osteonecrosis of the jaws: case-control study from the CONDOR Dental PBRN. Journal of Dental Research 2011; 90(4):439-444.
Data set-history (The data set link is best downloaded through Internet Explorer)
Data set-MDs (The data set link is best downloaded though Internet Explorer)
Study PI: Dr. Thomas Houston, University of Alabama at Birmingham
Brief Study Description
This was an internet-based clinical trial of oral cancer prevention. Eligibility required having internet access in the dental practice. The project was directed at prevention of oral cancer in dentistry by offering internet education and tools for the practice and support for all members of the practice. The project was not very time consuming, did not require training beforehand, and enhanced preventive care and risk management in the practice. To participate, you must have: (a) completed a series of internet continuing education modules; (b) encouraged your staff to support the project by also completing the modules; (c) designated a staff member to distribute 100 postcard surveys to patients at four different times for total of 400 postcards; (d) used the educational tools to enhance the preventive care in your practice. In addition to other benefits, the practice was paid an honorarium for its participation. Due to the success of the recruitment of this study, we increased the number of participants from 140 to 190. The goal of 190 practitioners was met. Any information that was provided is confidential and only reported in the aggregate. This project was funded by an R01 grant from NIDA and NIDCR (R01-DA-17971).
Key study publications:
Houston TK, DeLaughter KL, Ray MN, Gilbert GH, Allison JJ, Kiefe CI, Volkman JE for the National Dental PBRN Collaborative Group. Cluster-randomized trial of a web-assisted tobacco quality improvement intervention of subsequent patient tobacco product use: A national dental PBRN study. BMC Oral Health 2013; 13(1):13.
This study received primary funding by R01-DA-017971. Consequently, the responsibility for public access to data from this study lies with that grant.
Several instruments were used for data collection in this study. Initially, the patients at each dental practice were queried about whether the dentist asked or advised about tobacco use, the patient’s smoking status and willingness to participate in a telephone interview.
Each dental practice completed a baseline survey about the demographics and characteristics of its practice.
After participating in the web intervention directed at increasing tobacco control practices in dentistry, the practices were re-assessed.
At the end of the study, patients who agreed to participate were contacted about the status of their tobacco use and attempts to quit.
Dental practices completed a final survey that assessed how their dental practice changed tobacco cessation practices.
Study PI: Dr. Andreea Voinea-Griffin, University of Alabama at Birmingham (deceased)
Brief Study Description
There is great variation in caries diagnosis and management, with many dentists choosing a surgical approach rather than non-invasive treatment methods (“watchful monitoring” combined with prevention) for early caries. Approaches that delay placement of the first restoration may be a key source of improving the long-term effectiveness of dental care. This project focused on improving the quality of dental care by fostering movement of the latest scientific advances into daily clinical practice in the area of early caries treatment.
The aims of this project were to: (1) develop a patient handout to encourage patient acceptance of non-invasive treatment for early caries in permanent teeth and to increase dentists” use of non-invasive treatment; (2) quantify patient satisfaction with treatment options for early caries to quantify patient acceptance; and (3) quantify pre- and post-intervention caries stage at which dentists place the first restoration to determine the feasibility of the intervention.
This project entailed instrument development as well as a feasibility study that informed the design of a subsequent clinical trial in dental private practices. Semi-structured qualitative interviews with 30 patients and 10 dentists were conducted to develop the patient handout. Specific factors from pre-existing patient satisfaction surveys were used as quantitative tools. The handout was tested for readability and content structure. The study design was factorial, with patient satisfaction and handout assessment data from 300 surveyed patients diagnosed with early caries by participating dentists. The feasibility study design was longitudinal with pre- and post-intervention caries stage data from each participating DPBRN dentist collected from the practice assessment questionnaires. The 10 practitioners were recruited to participate in the study, based on their early caries treatment pattern and a stratified convenience sampling scheme that encouraged representation of minority dentists and patients.
Key study publications:
Mitchell ST, Funkhouser E, Gordan VV, Riley JL III, Makhija SK, Litaker MS, Gilbert GH, National Dental PBRN Collaborative Group. Satisfaction with dental care among patients who receive invasive or non-invasive treatment for non-cavitated early dental caries: findings from one region of the National Dental Practice-Based Research Network. BMC Oral Health 2017; 17(1):70.
This study was primarily funded by F32-DE-18592. Because of the small number of practitioners and patients in this study and the fact that they were all from a limited geographic area, it is not possible to provide a de-identified data set that does not risk being identifiable. Therefore, no public use data set is available.
In Phase I, practitioners were interviewed about their opinions on non-invasive caries treatment and patients’ preferences by using an interview script .
Non-invasive treatment patients were offered the opportunity to provide feedback during a telephone interview.
Based on information collected from patients and providers in Phase I, we designed a patient education brochure and “patient satisfaction with treatment for early caries” survey in Phase II. These two forms were handed to the patients who participated in the Phase III study.
Each practitioner kept track of how many patients received non-invasive treatment for early caries during the data collection period, along with how many of these agreed to participate in the study.
Before the final data collection in Phase III, practitioners participated in an individual training session.
For each patient, practitioners completed a data collection form and a caries risk assessment form.
Study PI: Dr. Donald Nixdorf, University of Minnesota
Brief Study Description
This was a nested case-control study in which DPBRN Study 17 patients who still had pain at 6 months and were seen by endodontic and orofacial pain experts. The primary goal of this study was to determine the proportion of patients with pain who would best be managed with traditional dental care compared to those who had a non-odontogenic source for their pain, so that treatment directed at the etiology of their pain would occur.
Key study publications:
Daline IH, Nixdorf DR, Law AS, Pileggi R, McEdward D, Massingale S, Sowell E, National Dental PBRN Collaborative Group. 3-year outcome of patients with persistent pain after root canal treatment: the National Dental Practice-Based Research Network. Journal of Endodontics 2020; accepted.
Nixdorf DR, Law AS, Lindquist K, Reams GJ, Cole E, Kanter K, Nguyen RHN, Harris DR, National Dental PBRN Collaborative Group. Frequency, impact and predictors of persistent pain following root canal treatment: a National Dental PBRN study. Pain 2016; 157(1):159-165.
Nixdorf DR, Law AL, John MT, Sobieh RM, Kohli R, Nguyen RH, National Dental PBRN Collaborative Group. Differential diagnoses for persistent pain after root canal treatment: a study in the National Dental Practice-Based Research Network. Journal of Endodontics 2015; 41(4):457-463.
Data set (The data set link is best downloaded through Internet Explorer. The data set contains both the baseline and follow-up studies)
Study PI: Dr. Thomas Houston, University of Alabama at Birmingham
Brief Study Description
Dental practices have advanced tobacco cessation by adopting a model of brief advice similar to that used by medical providers. DPBRN will do a randomized clinical trial designed to allow dental hygienists to provide additional tobacco cessation counseling with little additional marginal effort. This would be done using an internet-based referral to external resources. This system, termed “Refer2Quit”, will allow hygienists to refer patients to a patient education website and accompanying Quitline, while the patient is still in the dental office. Our overall goal is to advance science related to internet use in health services delivery by targeting dental hygienists. The intervention will also support subsequent brief counseling by providing feedback on the activities of patients to the practice through a secure server.
We had these specific aims:
- Test the hypothesis that the proportion of patients REFERRED to self-management resource websites would be larger in intervention practices compared to control practices.
- To test the hypothesis that the proportion of patients referred who GO to the patient self-management website would be larger in intervention practices compared to control practices.
- To test the hypothesis that the proportion of smokers who are referred who QUIT at six months would be larger among intervention compared to control because of the additional connectivity of the intervention.
This was done by randomizing 80 community-based dental practices into a clinical trial that contrasts the intervention with a paper-based “information prescription”.
Key study publication:
Ray MN, Funkhouser E, Williams JH, Sadasivam RS, Gilbert GH, Coley HL, Houston TK for the National Dental PBRN Collaborative Group. Smoking cessation e-referrals: a National Dental Practice-Based Research Network randomized controlled trial. American Journal of Preventive Medicine 2014; 46(2):158-165.
Data set 1 (Data set link is best downloaded through Internet Explorer)
Data set 2 (Data set link is best downloaded through Internet Explorer)
Data set 3 (Data set link is best downloaded through Internet Explorer)
Data set 4 (Data set link is best downloaded through Internet Explorer)
Data set 5 (Data set link is best downloaded through Internet Explorer)
To determine study eligibility practices returned the interest survey.
Annotated version of interest survey
Each dental practice completed a baseline survey on the demographics and characteristics of its practice.
After randomization, providers completed a qualitative survey and an online survey.
Annotated version of online survey
Patients who were referred and logged-on to the patient intervention site completed an online survey.
Annotated version of patient online survey
The dental practices completed a final survey to reassess their tobacco control practices and the patients completed a follow-up survey to assess their smoking status six months after registering on the quit smoking website.
Study PI: Dr. Gregg Gilbert, University of Alabama at Birmingham
Brief Study Description
The overarching goal of DPBRN is to impact the practice of dentistry and improve patient care. A critical issue is assessing whether the research conducted is achieving this goal. The three NIDCR-funded PBRNs (DPBRN, NWPRECEDENT, and PEARL), collectively known as the “Collaboration on Networked Dental and Oral Health Research” (CONDOR), have developed a strategy for assessing the impact of practice-based dental research on the PBRN practices and on the practice of dentistry in general. The strategy involves the development and use of a core questionnaire that includes several questions from each PBRN that have been extracted from questionnaires previously administered as part of their initial research program activities.
This project comprised the first administration of this Core Questionnaire with the purpose of assessing dental practice changes that may have occurred since the earlier administration of the individual questions within the separate networks. It also collected baseline information for the others. The Core Questionnaire were re-administered at later points in time. In this manner changes in practice over time and concurrent with research results dissemination were measured.
Key study publications:
McBride R, Lindblad A, Williams OD, Leroux B, Lemann M, Rindal DB, Botello-Harbaum M, Gilbert GH, Gillette J, Demko C for the CONDOR Collaborative Group. Measuring the impact of practice-based research networks on member dentists in the Collaboration on Networked Dental and Oral Health Research, CONDOR. Journal of Dentistry 2013; 41(5):393-403.
Botello-Harbaum MT, Curro FA, Rindal DB, Gilbert GH, Hilton TJ, Collie D, Craig RG, Lehman M, McBride R, Vena DA, Thompson V, Lindblad A for the CONDOR Collaborative Group. Information-seeking behaviors of dental practitioners in three practice-based research networks. Journal of Dental Education 2013; 77(2):152-160.
Data set (Data set link is best downloaded through Internet Explorer)
View the questionnaire.
Detailed report, overall and by region.
Graphical presentation of study findings, overall and by region.
Study PI: Dr. Gregg Gilbert, University of Alabama at Birmingham
Brief Study Description
The purpose of this study was to update the status of practices in the network with regard to these items: practice type (solo, group, public health, academic, other); percent of patients who are regular care seekers versus problem-oriented; whether the practice shares facilities or organizational structure with medical providers; percent of patients with certain chronic diseases; how commonly patients are referred to physicians for medical evaluations; electronic dental record usage and type of software; preferences for how to have study results communicated; rubber dam usage for endodontic procedures; utilization of dental staff for specific dental procedures; opinions about dental therapists and other expanded-function dental staff.
Key study publications:
Funkhouser E, Fellows JL, Gordan VV, Rindal DB, Foy PJ, Gilbert GH for the National Dental PBRN Collaborative Group. Supplementing online surveys with a mailed option to reduce bias and improve response rate: the National Dental PBRN. Journal of Public Health Dentistry 2014; 74(4):276-282.
Anabtawi MF, Gilbert GH, Bauer MR, Reams G, Makhija SK, Benjamin PL, Williams OD for the National Dental PBRN Collaborative Group. Rubber dam use during root canal treatment: findings from The Dental Practice-Based Research Network. Journal of the American Dental Association 2013; 144(2):179-186.
Blue CM, Funkhouser DE, Riggs S, Rindal DB, Worley D, Pihlstrom DJ, Benjamin PL, Gilbert GH for the National Dental PBRN Collaborative Group. Utilization of non-dentist providers and attitudes toward new provider models: findings from the National Dental Practice-Based Research Network. Journal of Public Health Dentistry 2013; 73(3):237-244.
Data set (Data set link is best downloaded through Internet Explorer)
View the questionnaire.
Annotated version of the questionnaire
Detailed report, overall and by region.
Graphical presentation of study findings, overall and by region.
Study PI: Dr. Valeria Gordan, University of Florida
Brief Study Description
The purpose of this project was to use data from “primary” restorations to assess how defects that may lead to failure develop over time, and to follow restorations placed in a practice-based setting for up to three years. The specific aims were to:
- quantify the annual and 3-year incidence of defects and replacement rates on restorations inserted as primary restorations;
- test the hypothesis that directly-placed composite restorations have a significantly higher 3-year incidence of defects and significantly higher replacement rate after 3 years compared to amalgam restorations;
- test the hypothesis that the 3-year replacement rate of restorations in permanent teeth of adolescents is significantly higher than that of restorations in adults. Criteria used to evaluate restorations over time will be the same as those employed in the DPBRN study of replacement restorations. Recall frequency was according to the schedule used in the practice where the restoration was placed. Patients were informed about the follow-up study as part of the informed consent procedure. If a patient sought treatment in a different practice, informed consent included permission to contact that practice for information related to restoration(s) in this longitudinal study.
Key study publications:
McCracken MS, Gordan VV, Litaker MS, Funkhouser E, Fellows JL, Shamp DG, Qvist V, Meral J, Gilbert GH for the National Dental PBRN Collaborative Group. A 24-month evaluation of amalgam and resin-based composite restorations: findings from the National Dental Practice-Based Research Network. Journal of the American Dental Association 2013; 144(6): 583-593.
Data set (The data set link is best downloaded through Internet Explorer)
Annotated data form for year 1
Detailed report, overall and by region
Graphical presentation of study findings, also overall and by region
Study PI: Dr. Sonia Makhija, University of Alabama at Birmingham
Brief Study Description
Although the progression of cavitated dental caries has slowed dramatically over the years, the prevalence of precavitated lesions has significantly increased; therefore, diagnosing and following these lesions has become an important part of daily clinical practice. There has been some debate on the best way to manage and treat these small lesions long-term. Some clinicians believe it is best to perform operative treatment and conserve tooth structure; whereas, other clinicians believe in managing it with preventive treatment, allowing the lesion the potential to remineralize or arrest over time. Limited literature is available for these “questionable” lesions and the reasons behind why clinicians are having difficulty diagnosing and treating them.
The aims of this study were to (1a) for unopened questionable occlusal carious lesions, test the hypothesis that the baseline clinical characteristics are significantly associated with change in caries status; and (1b) for opened questionable occlusal carious lesions, test the hypothesis that the clinical characteristics at baseline are significantly associated with caries depth.
These aims were met by performing a follow-up on the consecutive questionable occlusal carious lesions enrolled in “Prevalence of Occlusal Carious Lesions”. The study recorded the status of these lesions, if treatment changed,and the condition of the restoration or sealant, if applicable.
This study about occlusal carious lesions provided the opportunity to compare these results to “Assessment of Caries Diagnosis and Caries Treatment”, and “Prevalence of Occlusal Carious Lesions”.
Key study publication:
Makhija SK, Gilbert GH, Funkhouser E, Bader JD, Gordan VV, Rindal DB, Qvist V for the National Dental PBRN Collaborative Group. Twenty-month follow-up of occlusal caries lesions deemed questionable at baseline: findings from the National Dental Practice-Based Research Network. Journal of the American Dental Association 2014; 145(11):1112-1118.
Data set (Data set link is best downloaded through Internet Explorer)
Follow-up data collection form. Lesions were followed for 24 months.
Annotated follow-up data collection form
Detailed report, overall and by region
Graphical presentation of study findings, overall and by region.
Study PI: Dr. Valeria Gordan, University of Florida
Brief Study Description
The purpose of this project was to use data from the DPBRN study of replacement restorations to assess how defects that lead to failure develop over time, and follow restorations placed in a practice-based setting for up to three years.
The specific aims were to:
- quantify the annual and 3-year incidence of defects and replacement rates on restorations inserted as replaced restorations;
- test the hypothesis that directly-placed composite restorations have a significantly higher 3-year incidence of defects and significantly higher replacement rate after 3 years compared to amalgam restorations;
- test the hypothesis that there is no significant difference in 3-year replacement rates between restorations inserted that were partially replaced as compared to restorations that were completely replaced during DPBRN study of replaced restorations; and
- test the hypothesis that the 3-year replacement rate of restorations in permanent teeth of adolescents is significantly higher than that of restorations in adults.
Recall frequency was according to the schedule used in the practice where the restoration was placed. Patients were informed about the follow-up study as part of the informed consent procedure. If a patient sought treatment in a different practice, informed consent included permission to contact that practice for information related to restoration(s) in DPBRN longitudinal study.
Key study publication:
Gordan VV, Riley JL III, Geraldeli S, Williams OD, Spoto JC 3rd, Gilbert GH, National Dental PBRN Collaborative Group. The decision to repair or replace a defective restoration is affected by who placed the original restoration: findings from the National Dental PBRN. Journal of Dentistry 2014; 42(12):1528-1534.
Data set (The data set link is best downloaded through Internet Explorer)
Study PI: Dr. Joseph Riley, III, University of Florida
Brief Study Description
Patient satisfaction is important to practicing dentists because of links to regular return visits, caregiver trust, perception of technical competence, and treatment outcome. However, little is known about the satisfaction of dental patients, particularly as related to specific dental procedures. Dental restorations are one of the most commonly performed dental procedures, yet no study has documented patient satisfaction with a restoration-specific dental visit. There are many unique characteristics to a dental restoration visit such as dentist-patient communication about the restoration material, comfort during and following the procedure, and the patient’s view of the quality of the restoration. How patients prioritize these characteristics or use them in decisions about satisfaction are unknown. It is known that patients make judgments of the technical competence of dentists, but whether these judgments have any association with immediate or long-term restoration quality and therefore the extent to which they are valid is undetermined.
The aims of the study were to determine the relative contribution and importance of characteristics of a restoration and restoration visit with overall patient satisfaction following a dental visit that involved a restoration replacement or repair; and to link patient’s satisfaction and perception of the dentist’s technical expertise with long-term objective outcomes of the dental restoration.
This study involved approximately 6,000 patients that received at least one dental restoration repair/replacement. Patients were recruited from practices participating in the DPBRN study of replacement restorations, most of whom were enrolled in a DPBRN longitudinal study. Participants completed and mailed the survey questionnaire the day following the dental visit to allow them to evaluate and respond to the short-term outcomes, such as comfort and function, as well as to the immediate aspects of the visit.
Key study publications:
Riley JL III, Gordan VV, Hudak-Boss S, Fellows JL, Rindal DB, Gilbert GH for the National Dental PBRN Collaborative Group. Concordance between patient satisfaction and the dentist’s view: findings from the National Dental Practice-Based Research Network. Journal of the American Dental Association 2014; 145(4):355-362.
Riley JL III, Gordan VV, Rindal DB, Fellows JL, Qvist V, Patel S, Foy P, Williams OD, Gilbert GH for the National Dental PBRN Collaborative Group. Components of patient satisfaction with a dental restorative visit: results from The Dental Practice-Based Research Network. Journal of the American Dental Association 2012; 143(9):1002-1010.
Data set-dentist (The data set link is best downloaded through Internet Explorer)
Data set-patients (The data set link is best downloaded through Internet Explorer)
View the patient questionnaire.
The dentists who did the dental restoration at this visit also completed a questionnaire for each patient visit.
Detailed report, overall and by region.
Graphical presentation of study findings, overall and by region.
Study PI: Dr. Donald Nixdorf, University of Minnesota
Brief Study Description
Pain following root canal therapy occurs commonly, with an incidence range of 3% to 58% depending on the definition. The majority of this post-endodontic pain is well controlled using current treatment modalities, but a small subset of patients seems to be resistant to treatment and experiences severe pain. Significant post-endodontic pain is commonly referred to as an endodontic flare-up and has been defined as severe pain that precipitates a patient-dentist interaction within one week of treatment initiation. Such pain, when associated with local soft tissue swelling, is known to occur in 3% of all cases of root canal therapy. Given that >16.4 million root canal therapies are performed every year within the US, about half a million patients experience severe pain that is resistant to treatment. This pain is known to cause significant amounts of dental anxiety and fear, which in turn is a major barrier to receiving dental care and can have other negative psychosocial consequences. For these reasons, it is important to understand the factors related to the development of endodontic flare-up pain in efforts to better treat this pain. Research on endodontic-related pain has suggested that (a) the intensity of pre-operative pain and (b) the experience of intra-operative pain are significant factors related to the subsequent development of persistent tooth pain. Therefore, the primary goal of this study was to assess the presence and magnitude of pre-operative and intra-operative tooth pain, and determined how these factors were associated with the outcome of intense post-endodontic flare-up pain. The overall goal was to better understand how the experience of peri-operative pains relate to each other. The long-term goal of this line of research was to identify the modifiable pre-operative factors that put patients at greater risk of developing persistent tooth pain following root canal therapy, thereby providing evidence that will allow dentists to act preventively to mitigate this risk, improve pain control, increase their patients’ quality of life, and decrease the number of dental emergency interactions. Since future studies within the network are required to achieve this long-term goal, the secondary goal of this study was to assess the feasibility of recruiting patients using the DPBRN and to pilot test a more detailed data collection procedure from both patients and practitioners using a small subset of practitioners and within the DPBRN.
Key study publications:
Law AS, Nixdorf DR, Rabinowitz I, Reams GJ, Smith JA Jr., Torres AV, Harris DR, for the National Dental PBRN Collaborative Group. Root canal therapy reduces multiple dimensions of pain: a National Dental PBRN Study. Journal of Endodontics 2014; 40(11):1738-1745.
Nixdorf DR, Law AS, Look JO, Rindal DB, Durand EU, Kang W, Agee BS, Fellows JL, Gordan VV, Gilbert GH for the National Dental PBRN Collaborative Group. Large-scale clinical endodontic research within the context of The National Dental Practice-Based Research Network: study overview and methods. Journal of Endodontics 2012; 38(11):1470-1478.
Data set (The data set link is best downloaded through Internet Explorer. The data set contains both the baseline and longitudinal studies)
Practitioner completed a data form before beginning the root canal, and a different one after obturation.
Annotated forms for before beginning the root canal and after obturation.
Each practitioner also kept track of how many eligible patients presented for treatment during the data collection period, along with how many of these agreed to participate in the study.
Patients who were receiving root canal treatment completed a questionnaire immediately before treatment , another one immediately after treatment, and another form one week after treatment.
Annotated forms for immediately before treatment, immediately after treatment, and one week after treatment.
Patients also completed a form with contact information. When the root canal treatment required more than one visit, comparable forms were again completed by the dentist practitioner and the patient.
An additional form was completed by the dentist regarding pain and anxiety management for the treated tooth.
Detailed report, overall and by region.
Graphical presentation of study findings, also overall and by region.
Study PI: Dr. Donald Nixdorf, University of Minnesota
Brief Study Description
Dentists perform over 16.4 million root canal therapies every year in the United States (American Dental Association, 2002). Persistent tooth pain, which is pain present 6 months after root canal therapy, is known to occur following root canal therapy in a fashion similar to other post-surgical pains, such as phantom limb pain. Research in this area is limited, but suggests a frequency of occurrence of 3% to 12% for persistent post-root canal pain. Despite the commonality of root canal treatment, the occurrence and severity of persistent tooth pain and extent of interference with daily life from this condition has not been well studied in dental care populations. Adequate treatments for some of these pains are emerging, and early identification and treatment may improve prognosis, but the first step is to determine how widespread the problem is and how severely it affects dental patients. This knowledge is expected to influence patient and provider decisions about dental treatment and to facilitate the development of preventative treatment strategies, such as pre-emptive analgesia, aimed at reducing patients’ modifiable peri-operative risk factors. The long-term goal of this line of research is to identify pre-operative factors that put patients at greater risk for developing persistent tooth pain following root canal therapy, thereby providing evidence that will allow dentists to act preventively to mitigate this risk, improve pain control, and increase their patients’ quality of life. For this long-term goal to be realized, future externally funded research using the DPBRN is anticipated; hence, there is a need for pilot data to support the feasibility of such research. Even though this research proposal is focused on understanding the outcomes of root canal therapy, with the long-term goal of improving care, the resultant data may have ramifications for surgical procedures performed elsewhere in the body. Undoubtedly aspects of this research will be specific to root canal therapy, but since pain is a centrally derived phenomenon that affects the whole individual, aspects of the involved pain mechanisms are likely shared with other surgical procedures. Thus, this line of research could have an impact on healthcare in general.
Key study publications:
Nixdorf DR, Law AS, Lindquist K, Reams GJ, Cole E, Kanter K, Nguyen RHN, Harris DR, National Dental PBRN Collaborative Group. Frequency, impact and predictors of persistent pain following root canal treatment: a National Dental PBRN study. Pain 2016; 157(1):159-165.
Nixdorf DR, Law AL, John MT, Sobieh RM, Kohli R, Nguyen RH, National Dental PBRN Collaborative Group. Differential diagnoses for persistent pain after root canal treatment: a study in the National Dental Practice-Based Research Network. Journal of Endodontics 2015; 41(4):457-463.
Law AS, Nixdorf DR, Aguirre AM, Reams GJ, Tortomasi AJ, Manne BD, Harris DR, National Dental PBRN Collaborative Group. Predicting severe pain after root canal therapy in the National Dental PBRN. Journal of Dental Research 2015; 94(3 Suppl) 37S-43S.
Data set (Data set link is best downloaded through Internet Explorer)
Patients were followed for six months after they completed treatment in the study ”Peri-operative pain and root canal therapy”, and were asked to return a three-month form and a six-month form.
Annoted three-month and six-month forms
Detailed report, overall and by region
Graphical presentation of study findings, overall and by region
Study PI: Dr. Gregg Gilbert, University of Alabama at Birmingham
Brief Study Description
The overarching goal of DPBRN is to impact the practice of dentistry and improve patient care. A critical issue is assessing whether the research conducted is achieving this goal. The three NIDCR-funded PBRNs (DPBRN, NWPRECEDENT, and PEARL), collectively known as the “Collaboration on Networked Dental and Oral Health Research” (CONDOR), developed a strategy for assessing the impact of practice-based dental research on the PBRN practices and on the practice of dentistry in general. The strategy involved the development and use of a core questionnaire that included several questions from each PBRN that have been extracted from questionnaires previously administered as part of their initial research program activities. This project comprised the pre-planned second administration of this Core Questionnaire with the purpose of assessing dental practice changes that may have occurred since the first administration (DPBRN Study 16).
Key study publications:
Norton WE, Funkhouser E, Makhija SK, Gordan VV, Bader JD, Rindal DB, Pihlstrom DJ, Hilton TJ, Frantsve-Hawley J, Gilbert GH for the National Dental PBRN Collaborative Group. Concordance between clinical practice and published evidence: findings from the National Dental Practice-Based Research Network. Journal of the American Dental Association 2014; 145(1):22-31.
Data set (The data set link is best downloaded through Internet Explorer)
View the questionnaire.
Detailed report, overall and by region.
Graphical presentation of study findings, overall and by region.
Study PI: Dr. Gregg Gilbert, University of Alabama at Birmingham
This was a retrospective cohort study to test the hypothesis that endodontic treatment failure is significantly higher among dental patients with diabetes mellitus type II when compared to non-diabetic controls. The idea for this research project was a result of ideas provided by dentists who completed the Dental PBRN enrollment questionnaire. This project was primarily funded by an R21 grant from NIDCR (R21-DE-16033).
Brief study description:
We have an innovative opportunity to develop the nation’s only dental practice-based research network, which is called the Alabama Dental Practice Research Network.
Specific Aim 1 was to enhance the infrastructure and research capacity of the network. This aim was accomplished by enhancing the administrative structure of the network, by providing fundamental training in clinical research and human subjects precautions to network dentists, and by providing a communication infrastructure for network practices and the network administration, which will include an internet-based system.
Specific Aim 2 was to conduct a feasibility study to test data collection methods for a retrospective cohort study that tested the hypothesis that endodontic treatment (root canal) failure was significantly higher among dental patients with diabetes mellitus type 2 when compared to non-diabetic controls.
This feasibility study provided a sound scientific foundation for an R01 application to investigate the potentially bi-directional relationship between diabetes mellitus type 2 and endodontic treatment failure, allowing us to determine whether diabetes contributes to poor endodontic healing, and whether inadequate endodontic healing can itself contribute to poor diabetic control.
Key study publication:
Gilbert GH, Tilashalski KR, Litaker MS, McNeal SF, Boykin MJ, Kessler AW for The DPBRN Collaborative Group. Outcomes of root canal treatment in Dental PBRN practices. General Dentistry 2010; 58(1): 28-36.
This study received primary funding by R21-DE-016033 (Alabama Dental Practice-Based Research Network Development). Consequently, the responsibility for public access to data from this study lies with that grant.
Study PI: Dr. Sonia Makhija, University of Alabama at Birmingham
Brief Study Description
Although the progression of cavitated dental caries has slowed dramatically over the years, the prevalence of precavitated lesions has significantly increased; therefore, diagnosing these lesions has become an important part of daily clinical practice. Due to the size of these lesions, the ability to correctly diagnose and treat them can be difficult. There has been some debate on the best way to manage and treat these small lesions. Some clinicians believe it is best to perform operative treatment and conserve tooth structure; whereas, other clinicians believe in managing it with preventive treatment, allowing the lesion the potential to remineralize or arrest. Limited literature is available for these “questionable” lesions and the reasons behind why clinicians are having difficulty diagnosing and treating them.
The aims of this study were to (1) quantify the prevalence of questionable occlusal carious lesions in permanent teeth in the first 100 consecutive eligible patients of DPBRN practitioners; (2a) for unopened questionable occlusal carious lesions, test the hypothesis that the patient’s baseline caries risk is significantly associated with lesion description (i.e., perceived caries status); and (2b) for opened questionable occlusal carious lesions, test the hypothesis that the patient’s baseline caries risk is significantly associated with caries depth.
These aims were met by enrolling 80-100 practitioner-investigators, each of whom recorded information about 100 consecutive patients and 25-50 consecutive questionable early occlusal caries lesions on a 2-page questionnaire. The study recorded the reason why these occlusal lesions were questionable, the tools used to diagnose the lesions, the reason why a certain treatment was rendered, and the depth of the lesions when treated operatively.
This study about early occlusal caries lesions provided the opportunity to compare these results to DPBRN study entitled “Assessment of Caries Diagnosis and Caries Treatment”, a questionnaire wherein practitioners’ caries diagnosis, caries treatment, and preventive dentistry practices were quantified as well as compare these results to the DPBRN study entitled “Longitudinal Study of Questionable Occlusal Carious Lesions”.
Key study publication:
Makhija SK, Gilbert GH, Funkhouser E, Bader JD, Gordan VV, Rindal DB, Pihlstrom DJ, Qvist V for the National Dental PBRN Collaborative Group. Characteristics, detection methods, and treatment of questionable occlusal caries lesions: findings from the National Dental Practice-Based Research Network. Caries Research 2014; 48(3):200-207.
Makhija SK, Gilbert GH, Funkhouser E, Bader JD, Gordan VV, Rindal DB, Bauer M, Pihlstrom DJ, Qvist V for the National Dental PBRN Collaborative Group. The prevalence of questionable occlusal caries lesions: findings from The Dental PBRN. Journal of the American Dental Association 2012; 143(12):1343-1350.
Data set (The data set link is best downloaded through Internet Explorer. The data set contains both the baseline and follow-up studies)
Annotated change of treatment form
Detailed report, overall and by region
Graphical presentation of study findings, overall and by region
Study PI: Dr. Eric Schiffman, University of Minnesota
Brief Study Description
The overall goal of this project was to collect data to be used in preparing an application for a Clinical Trial Planning Grant and then in designing a subsequent Phase III clinical trial. The ultimate goal was to determine the most practical approach to conduct a randomized clinical trial to evaluate initial interventions for patients with painful temporomandibular muscle and joint disorders (TMJD) in primary care clinics. This project characterized by surveying the feasibility of recruiting dentists in primary care dental clinics in The Dental Practice-Based Research Network and document their current initial care for their TMJD pain patients.
Key study publication:
Velly AM, Schiffman EL, Rindal DB, Cuhna-Cruz J, Gilbert GH, Lehmann M, Horowitz A, Fricton J, McBride R for the CONDOR Collaborative Group. The feasibility of clinical trial of pain related to temporomandibular muscle and joint disorders: The results of a survey from the Collaboration on Networked Dental and Oral Research dental practice-based research networks. Journal of the American Dental Association 2013; 144(1):e01-e10.
Data set (Data set link is best downloaded through Internet Explorer)
View the questionnaire.
Detailed report, overall and by region.
Graphical presentation of study findings, overall and by region.
Study PI: Dr. Valeria Gordan, University of Florida
Brief Study Description
This study of previously-untreated permanent tooth surfaces was the second of the restorative dentistry studies planned for the Dental Practice-Based Research Network (DPBRN). The aims for this study were to: (a) quantify DPBRN practitioner-investigators’ pre-operative and post-operative assessments of the depth of the caries lesion being treated and (b) quantify the prevalence of dental material types used to restore the first restoration in a permanent tooth surface. These aims were met by enrolling 229 DPBRN practitioner-investigators in this study, each of whom recorded information about an average of 50 consecutive restorations that they placed on unrestored permanent tooth surfaces. The study recorded the main reason that the restoration was placed, the preoperative and postoperative depth of the caries lesion on the previously unrestored surface, and the type of dental restorative material that was used. This study about restorative treatment received by DPBRN patients provided the opportunity to record not only the diversity in the treatment provided, but also to generate information for subsequent hypothesis testing and for the design of future studies.
Key study publications:
Nascimento MM, Bader JD, Qvist V, Litaker MS, Williams OD, Rindal DB, Fellows JL, Gilbert GH, Gordan VV for The DPBRN Collaborative Group. Concordance between pre-operative and post-operative assessments of primary caries lesion depths: results from The Dental PBRN. Operative Dentistry 2010; 35(4): 391-398.
Nascimento MM, Gordan VV, Qvist V, Litaker MS, Rindal DB, Williams OD, Fellows JL, Ritchie LK Jr, Mjör IA McClelland J, Gilbert GH for The DPBRN Collaborative Group. Reasons for placement of restorations on previously un-restored tooth surfaces by dentists in The Dental Practice-Based Research Network. Journal of the American Dental Association 2010; 141(4): 441-448.
Data set (The data set link is best downloaded in Internet Explorer. The data set consists of the baseline and follow-up studies)
Detailed report, overall and by region
Graphical presentation of study findings, overall and by region.
Study PI: Dr. Valeria Gordan, University of Florida
Brief Study Description
This study recorded the reason(s) for replacement or repair of 50 consecutive restorations as diagnosed by 200 DPBRN clinicians. This constituted baseline data which was used for analysis of factors that affect the diagnoses.
Factors that affected the number of replaced or repaired restorations was analyzed using baseline data, e. g., how they vary among clinicians, the practice setting, the gender of the patients and the clinicians, and the clinicians” attitudes towards caries lesion development and caries risk assessment. These data was also a source for monitoring treatment changes in restorative dentistry that may occur over time. A better understanding of the reasons why restorations needed to be replaced or repaired led to improvements in the longevity of restorations.
Key study publications:
Gordan VV, Riley JL III, Worley DC, Gilbert GH for The DPBRN Collaborative Group. Restorative material and other tooth-specific variables associated with the decision to repair or replace defective restorations: findings from The Dental PBRN. Journal of Dentistry 2012; 40(5):397-405.
Gordan VV, Riley JL III, Geraldeli S, Rindal DB, Qvist V, Fellows JL, Kellum HP, Gilbert GH for the National Dental PBRN Collaborative Group. Repair or replacement of defective restorations by dentists in The Dental Practice-Based Research Network. Journal of the American Dental Association 2012; 143(6):593-601.
Data set (The data set link is best downloaded through Internet Explorer. The data set consists of the baselind and follow-up studies)
Each practitioner kept track of how many eligible patients presented for treatment during the data collection period, along with how many of these agreed to participate in the study.
Each practice kept track of the names of each participant because the network tracked these restorations longitudinally. This information was kept at the dental practice and at the regional office, but was not passed on to the Coordinating Center.
Detailed report, overall and by region.
Graphical presentation of study findings, also overall and by region.
Study PI: Dr. Jeffrey Fellows, Kaiser Permanente Center for Health Research
Brief Study Description
In the past two years, the literature has described more than 200 cases of osteonecrosis of the jaws (ONJ) among patients treated with bisphosphonates (BPs). About 3 million patients have been treated with BPs and another 7-8 million osteoporotic or cancer-afflicted persons in the U.S. may take BPs in the near future. To date, the prevalence of ONJ has not been quantified, nor is it known whether exposure to BPs actually increases ONJ prevalence. We investigated these issues using data from a large cohort of patients from the Kaiser Permanente Northwest and HealthPartners medical and dental plans. Both health maintenance organizations are part of DPBRN, allowing us to take advantage of an already-functioning interdisciplinary collaborative infrastructure.
This study addressed three specific aims. Aim 1 quantified the annual, consecutive prevalence of confirmed ONJ cases in a large cohort of adults 40 years of age and older from 1994 to 2005. Aim 2 tested the hypothesis that BP treatment is a risk factor for ONJ. We quantified the impact of BP exposure on the risk of developing ONJ, relative to comparable patients not exposed to BP, using a retrospective cohort design and time-to-event analysis. Finally, Aim 3 tested the hypothesis that ONJ develops only in patients treated with BPs who have additional risk factors. These health maintenance organizations provided a unique, unprecedented opportunity to investigate ONJ by including thousands of patients through their electronic medical and dental records.
Relevance to public health: In light of the substantial morbidity due to ONJ, this study provided important information about this growing health concern.
Key study publication:
Fellows JL, Rindal DB, Barasch A, Gullion CM, Rush W, Pihlstrom DJ, Richman J for The DPBRN Collaborative Group. ONJ in two Dental Practice-Based Research Network regions. Journal of Dental Research 2011; 90(4):433-438.
Data set (Data set link is best downloaded through Internet Explorer)
Read about the the following study highlights from the Practice-Based Research Network:
- Assessing Outcomes of Cracked Teeth
- Remineralization of White Spot Lesions after Removal of Orthodontic Brackets
- Single Tooth Endodontic and Restorative Treatment Outcomes: PEARL Interim Findings
- PEARL Non-Carious Cervical Lesion RCT Baseline and Sleep Bruxism Findings
- Lessons Learned During the Conduct of Clinical Studies in the Dental PBRN
- Repair or Replacement of Defective Restorations by Dentists in the Dental PBRN